Acupuncture combined with antidepressants is safe and effective for the treatment of depression. A meta-analysis of thirteen quality randomized-controlled trials published in the Journal of Affective Disorders finds acupuncture combined with antidepressant therapy is “more effective than antidepressants alone….” The therapeutic effects of the combination are rapid and the data finds acupuncture effective in reducing the adverse effects associated with antidepressant medications. 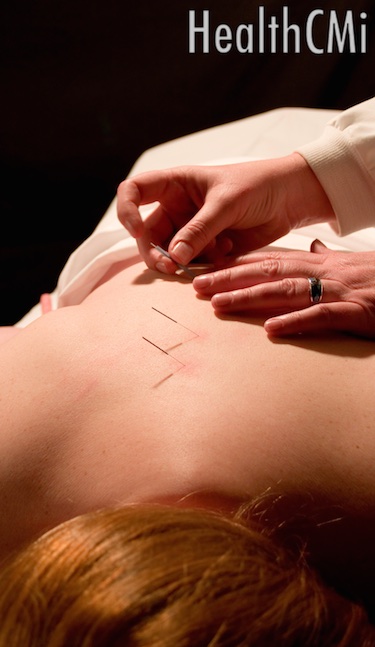
Researchers note, “This meta-analysis reveals clear evidence of greater antidepressant activity with acupuncture combined with a(n) SSRIs compared with SSRIs alone….” SSRIs (selective serotonin reuptake inhibitors) are a class of antidepressants that increase levels of serotonin in the brain. The researchers note that acupuncture has been shown to stimulate neurotransmitters in the brain thereby increasing serotonin and norepinephrine levels. They add that acupuncture increases the “activity of serotonergic neurons in the reward system pathway of the brain.” They note, “Acupuncture treatments have also been shown to increase nocturnal melatonin secretion and reduce insomnia and anxiety.”
The researchers note that acupuncture’s ability to increase opiod peptides in the body may account for its ability to provide rapid relief from depression. They note, “acupuncture is capable of rapidly increasing the bodily release of endogenous opioid peptides associated with the production of pleasure and relief of anxiety and gastrointestinal discomfort.”
The researchers cite laboratory research finding electroacupuncture and manual acupuncture effective in relieving depression. Real-time polymerase chain reaction genomic research confirms that acupuncture normalizes a broad spectrum of gene expression, decreases damage to hippocampal neurons, and regulates “serum levels of corticosterone and adrenocorticotropic hormone.” The researchers note that “acupuncture may treat depression by influencing the neuroendocrine and immune systems through the regulation of levels of serotonin, norepinephrine, dopamine, endorphins and glucocorticoids…, stimulating hypothalamic and hippocampal responses…, and by regulating the expression of certain genes.”
The researchers note that acupuncture may be an effective standalone treatment modality for partial responders and nonresponders to antidepressant medications. Citing Wu et al., they note “that acupuncture has the potential to be an effective, safe and well-tolerated monotherapy for depression and a viable augmentation agent for partial responders and nonresponders to antidepressant treatment.” They add that two other meta-analyses confirm these findings citing that acupuncture “significantly reduces depressive severity” and is safe and effective for post-stroke depression patients.
The researchers analysed the trials and determined a set of acupuncture points that were most commonly used across all of the studies:
Baihui (GV20)
Yintang (EX-HN3)
Shenmen (HT7)
Sanyinjiao (SP6)
Hegu (LI4)
Neiguan (PC6)
Dazhui (GV14)
Sishencong (EX-HN1)
Shenting (GV24),
Fengfu (GV16)
Fengchi (GB20)
Topping the list for the most common points across all studies were acupuncture points GV20 and Yintang. The total sample size was 1,046 human subjects. The total number of acupuncture treatments ranged between 9 and 36. The majority of participants received acupuncture in the course of a six week treatment window.
Acupuncture provides significant advantages to those taking antidepressant medications by reducing adverse effects. The researchers find acupuncture effective in reducing nausea, weight gain and sexual disorders associated with antidepressant medication intake.
 The researchers summarize, “combining acupuncture with antidepressant treatment may ameliorate depressive symptoms as well as control antidepressant side effects.” The researchers note that the data indicates that combining acupuncture and pharmacotherapy creates an additive effect; the total therapeutic effect is the sum of the two treatments added together.
The researchers summarize, “combining acupuncture with antidepressant treatment may ameliorate depressive symptoms as well as control antidepressant side effects.” The researchers note that the data indicates that combining acupuncture and pharmacotherapy creates an additive effect; the total therapeutic effect is the sum of the two treatments added together.
Reference:
Chan, Yuan-Yu, Wan-Yu Lo, Szu-Nian Yang, Yi-Hung Chen, and Jaung-Geng Lin. "The benefit of combined acupuncture and antidepressant medication for depression: A systematic review and meta-analysis." Journal of Affective Disorders (2015).


