Acupuncture suppresses epilepsy and benefits sleep. Researchers tested electroacupuncture in a laboratory experiment to determine the effects of low-frequency (10 Hz) simulation of acupoint GB20 (Fengchi) on epilepsy. 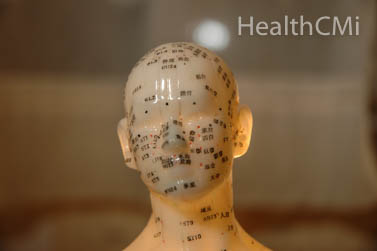 Electroencephalogram (EEG) results demonstrate that electroacupuncture significantly suppresses brain epileptiform discharges and simultaneously improves sleep patterns. In addition, the researchers discovered a biochemical mechanism responsible for acupuncture’s therapeutic effects.
Electroencephalogram (EEG) results demonstrate that electroacupuncture significantly suppresses brain epileptiform discharges and simultaneously improves sleep patterns. In addition, the researchers discovered a biochemical mechanism responsible for acupuncture’s therapeutic effects.
The researchers note that acupuncture’s ability to reduce epilepsy and associated sleep disruptions has important therapeutic implications. The researchers state that a procedure that suppresses epilepsy and improves sleep is “optimal for seizure control.” The modern research has an historical basis. The investigators note that an ancient Chinese classic, the Lingshu Jing, documents acupuncture’s ability to suppress epileptic seizures and reduce insomnia. This modern experiment confirms principles and indications written in the Lingshu Jing, the Spiritual Pivot.
Citing both clinical and experimental investigations, the researchers note that “epilepsy and sleep reciprocally influence each other.” They add that temporal lobe related epilepsy is related to sleep fragmentations and decreases in sleep efficiency. Frontal lobe related epilepsy is related to “sleep instability and arousal fluctuations.” Rapid eye movement (REM) “sleep decreases seizure susceptibility.” The lab experiment demonstrates that acupuncture improves sleep while simultaneously suppressing epilepsy.
The research demonstrates that 10 Hz electroacupuncture and not 100 Hz electroacupuncture is effective for the suppression of epilepsy. The researchers note, “The choice of frequency for EA (electroacupuncture) stimulation is an important issue in order to exert a therapeutic effect.” The researchers note that low frequency stimulation of GB20 suppresses epilepsy and “blocks sleep disruption….” In addition, the laboratory results demonstrate that opioid receptors mediate the effects of electroacupuncture stimulation.
The investigators cite research showing that opioid peptides and their receptors mediate the therapeutic effects of acupuncture. Han et al. demonstrate that 2 Hz electroacupuncture stimulates increases of met-enkephalin but not dynorphin. However, 100 Hz electroacupuncture increases dynorphin release and not met-enkephalin. Administration of naloxone, an opiod receptor antagonist, to the laboratory rats in the epilepsy experiment blocked the ability of electroacupuncture to suppress epilepsy. The researchers add that this is “consistent with the results that indicate naloxone blocks the morphine-induced anticonvulsant effect.” Naloxone also blocked 10 Hz electroacupuncture’s ability to improve sleep in the experiment’s epileptic rats. The researchers note that this indicates that opiod receptors mediate the therapeutic responses of electroacupuncture on the suppression of epilepsy and related sleep concerns.
Yi et al. review important statistics regarding epilepsy. The investigators indicate that 70% of epilepsy cases “can be controlled by current anti-epileptic drugs (AEDs); however, seizures recur in 30% of patients who do not respond to any of the first-line AEDs despite administration of the optimized dosage.” Also, a disruption of sleep “deteriorates and worsens the progression of epilepsy.” The new research indicates that low frequency electroacupuncture demonstrates important therapeutic implications for patients with epilepsy and epilepsy related sleep disorders. 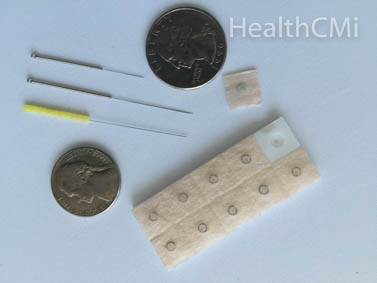
In related research, investigators from the Ninth People’s Hospital of Henan randomly divided 60 patients with epilepsy into a control group and an acupuncture group. The control group received only the pharmaceutical medication sodium valproate. The acupuncture group received both scalp acupuncture and body acupuncture plus sodium valproate. The acupuncture group demonstrated significantly superior patient outcomes over the medication only group.
Scalp acupuncture was applied to the chest area, the epilepsy-control area and the chorea-tremor control area. Body style acupuncture was applied to:
- Fengchi (GB20)
- Baihui (DU20)
- Sishencong (EX-HN1)
- Yintang (EX-HN3)
- Shuigou (DU26)
- Neiguan (PC6)
- Hegu (LI4)
- Zusanli (ST36)
- Fenglong (ST40)
- Sanyinjiao (SP6)
- Taichong (LR3)
The lifting and thrusting needle technique was applied to DU26, PC6, Yintangs, DU20, Sishencong, and LI4. The reinforcing-reducing method was applied to other acupoints until the patient experienced the arrival of deqi. The needles were retained for 30 minutes. A total of 10 days comprised one course of care. There was a 2 day break following each course of care. The treatment period was 3 months.
Following the completion of acupuncture therapy, a total of 12 acupuncture patients showed no epilepsy related symptoms for at least 1 year. A total of 9 patients showed excellent improvements and 6 patients showed moderate improvements. The overall effective rate for the acupuncture group was 90.00% compared with 73.33% for the medication control group. The researchers concludes that acupuncture combined with sodium valproate has a synergistic clinical effect leading to improved patient outcomes.
Ear And Scalp Acupuncture
Lin et al. conducted a laboratory experiment on two types of acupuncture that were each successful in halting epileptic seizures. Auricular acupuncture and body style electroacupuncture reduced neuron overexcitation while simultaneously stopping epileptic seizures. The researchers quantified acupuncture’s ability to regulate the TRPA1 ion signalling channel located on the plasma membrane of cells. The TRPA1 protein-coding gene is active in acute pain and neurogenic inflammation. Auricular and electroacupuncture demonstrate the ability to halt inflammation related to epileptic seizures while simultaneously downregulating TRPA1 in the hippocampus. Results were confirmed by western blot analysis, EEG, and electromyogram (EMG) techniques.
The auricular acupuncture group received 2 Hz electroacupuncture stimulation from the ear apex to the ear lobe for 20 minutes on the left ear and 10 minutes on the right ear per session. The body style electroacupuncture group received 2 Hz electroacupuncture from acupoints ST36 (Zusanli) to ST37 (Shangjuxu). Both groups received acupuncture at a rate of 3 days per week for a total of 6 weeks. Auricular and body style acupuncture were effective in providing relief from epileptic seizures and both types of acupuncture regulated the TRPA1 signaling pathway and additional signalling pathways: PKC, pERK1/2. The researchers note, “These novel findings are remarkable and compelling and reveal the crucial curative effects of auricular EA (electroacupuncture).”
References:
Yi, Pei-Lu, Chin-Yu Lu, Shuo-Bin Jou, and Fang-Chia Chang. "Low-frequency electroacupuncture suppresses focal epilepsy and improves epilepsy-induced sleep disruptions." Journal of biomedical science 22, no. 1 (2015): 1-12.
Fei H, Xie GX, Han JS. Low and high frequency electroacupuncture stimulation release [Met] enkephalin and dynorphin A in rat spinal cord. Sci Bull China. 1987;32:1496–501.
Bazil CW. Sleep and epilepsy. Semin Neurol. 2002;22:321–7.
Niu, Xuexia. “Clinical observation on treating 30 cases of epilepsy by head and body acupuncture.” Clinical Journal of Chinese Medicine 6.4 (2014): 65-67.
Lin, Yi-Wen, and Ching-Liang Hsieh. "Auricular Electroacupuncture Reduced Inflammation-Related Epilepsy Accompanied by Altered TRPA1, pPKCα, pPKCε, and pERk1/2 Signaling Pathways in Kainic Acid-Treated Rats." Mediators of Inflammation 2014 (2014).


