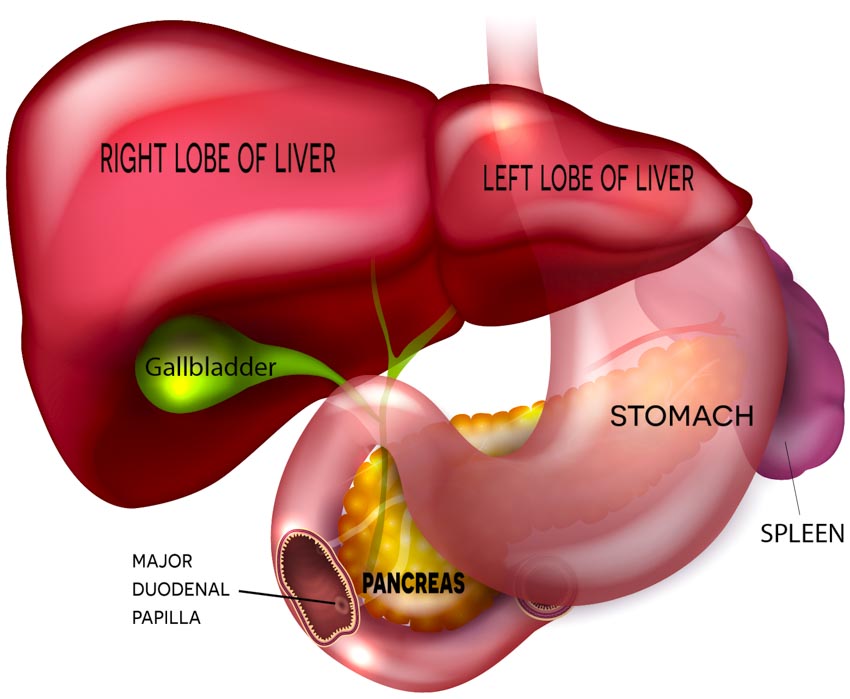
Researchers find acupuncture and herbs effective for the treatment of liver cirrhosis. Researchers from the Third People’s Hospital of Yiwu City combined acupuncture and herbs with standard drug therapy. Patients receiving both drug therapy and TCM (Traditional Chinese Medicine) treatment in a combined treatment protocol had superior patient outcomes compared with patients receiving only drug therapy. The researchers conclude that the addition of acupuncture and herbs to conventional drug therapy can “effectively improve liver function, control the development of the disease, promote the recovery of gastrointestinal function, and reduce relevant complications.” [1]
Multiple subjective and objective instruments were used to measure patient outcomes. First, liver fibrosis markers were measured, including laminin (LN), hyaluronic acid (HA), and type-III procollagen (PCⅢ). Second, gastrointestinal symptoms were evaluated using the gastrointestinal symptom scale. Higher gastrointestinal symptom scores are associated with worsening gastrointestinal symptoms. Third, liver function markers were recorded, including albumin (ALB), total bilirubin (TBil), alanine transaminase (ALT), and aspartate transaminase (AST).
Fourth, the prognosis of liver cirrhosis was calculated using the Child-Pugh score. Higher Child-Pugh scores are associated with poorer prognoses. Fifth, the recovery of gastrointestinal function was quantified by measuring recovery time of bowel sounds, end time of regurgitation and vomiting, and daily defecation frequency. Sixth, the incidence rate of complications (ascites, pleural effusion, edema of both lower extremities, abdominal varicose veins) in the two groups were compared.
After treatment, liver fibrosis markers (LN, HA, PCⅢ) and gastrointestinal symptom scores improved significantly in the two groups (p<0.01). Liver fibrosis markers, gastrointestinal symptom scores, liver function markers (ALT, ALB, AST, TBil), Child-Pugh scores, and gastrointestinal functions in the TCM treatment group were significantly better than those in the drug monotherapy control group (p<0.01). In addition, the TCM treatment group had a 10.7% complication rate, while the drug monotherapy control group had a 38.2% complication rate (p<0.05).
Design
Researchers (Li et al.) used the following study design. A total of 62 patients were treated and evaluated in this study. They were all selected from the Third People’s Hospital of Yiwu City. They were randomly divided into an acupuncture and herbs treatment group and a drug monotherapy control group, with 28 and 34 patients in each group respectively. For the control group patients, conventional drug therapy was administered. The treatment group received acupuncture and herbs in addition to the identical drug therapy administered to the drug control group.
The statistical breakdown for each randomized group was as follows. The treatment group was comprised of 10 males and 18 females. The average age in the treatment group was 41 years. The average course of disease in the treatment group was 5.16 years. The control group was comprised of 12 males and 22 females. The average age in the control group was 41 years. The average course of disease in the control group was 5.16 years. There were no significant statistical differences in gender, age, and course of disease relevant to patient outcome measures for patients initially admitted to the study. For both groups, patients received the following conventional drug therapy:
- Drugs to alleviate jaundice and protect liver function
- Drugs to relieve portal hypertension
- Intravenous therapy to correct fluid, electrolyte, and acid-base disorders
- Nutritional support
- Adefovir dipivoxil capsules were prescribed for viral liver cirrhosis
- Serum albumin (ALB) was prescribed for severe conditions
TCM Treatment
The treatment group patients received acupuncture and herbs in addition to drug therapy. The following acupoints were selected bilaterally for the treatment group:
- ST25 (Tianshu)
- ST36 (Zusanli)
- ST37 (Shangjuxu)
- ST39 (Xiajuxu)
- CV4 (Guanyuan)
- CV12 (Zhongwan)
Acupuncture treatments commenced with patients in a supine position. After disinfection of the acupoint sites, a 0.30 mm × 40 mm disposable filiform needle was inserted into each acupoint with a high needle entry speed. A deqi sensation was obtained and the needles were manually stimulated with Ping Bu Ping Xie (mild attenuating and tonifying) manipulation techniques. The needles were retained for 30 minutes. Acupuncture sessions were administered once per day, for a total of 30 consecutive days. The herbal formula used in this study (modified Si Jun Zi Tang) contained the following ingredients:
- Huang Qi 30 grams
- Tai Zi Shen 30
- Ze Xie 15
- Da Fu Pi 15
- Fu Ling 12
- Sang Bai Pi 10
- Chao Bai Zhu 10
- Gan Cao 3
Additional herbs were prescribed based on differing diagnostic patterns. For blood stasis in the liver and spleen, the following herbs were added:
- Xian He Cao 30 grams
- Dan Shen 20
- Bie Jia 15
- Di Yu 15
- Huai Hua 15
For damp-heat brewing and binding, the following herbs were added:
- Ji Gu Cao 30 grams
- Mian Yin 20
- Bai Hua She She Cao 20
For qi stagnation and damp obstruction, the following herbs were added:
- Mai Ya 30 grams
- Sha Ren 10
- Hou Po 10
- Chen Pi 8
For cold-damp encumbering the spleen, the following herbs were added:
- Mu Gua 10 grams
- Gan Jiang 6
- Cao Guo Ren 6
- Mu Xiang 6
The researchers note that the ingredients benefit the spleen and liver, free the channels, drain pathogenic water, accelerate blood circulation, and help the body to remove blood stasis. The prescribed dosage was one decoction daily. The above ingredients were brewed with water to obtain a 350 ml decoction, which was then split into 2 servings, taken separately in the morning and at night. Patients consumed the TCM herbal medicine at this rate for 30 consecutive days.
Results
The results indicate that acupuncture and herbs combined with drug therapy into an integrated treatment protocol is more effective than drug monotherapy. Li et al. conclude that acupuncture and herbs are safe and effective for the relief of liver cirrhosis.
Reference:
[1] Li J, Luo JC, Fu HM, Chen H, Feng LM. Clinical Study on Acupuncture plus Si Jun Zi Decoction in Treating Hepatocirrhosis [J]. Shanghai Journal of Acupuncture and Moxibustion, 2019,38(04):369-373.


