Acupuncture and Chinese herbal medicine improve patient outcomes for patients with acute or chronic appendicitis. Jining City Municipal Hospital (Shandong) researchers tested two protocols. One group received usual care, and another received usual care plus the addition of acupuncture and Chinese herbal medicine. The acupuncture and herbal medicine group had a 94.44% effective rate compared with 89.47% in the usual care group. [1] Importantly, the addition of acupuncture and herbal medicine resulted in shorter hospitalization durations, faster resolution of abdominal pain, and faster regulation of body temperatures.
A total of 38 patients with acute appendicitis were recruited for the study and were randomly assigned to the acupuncture and herbs group or the usual care group. One patient from the acupuncture and herbs group did not complete treatment, leaving complete data for 18 patients. The group was comprised of 9 male and 10 female patients, ages 18–62 years (mean age 42.34 years). Patients were admitted to the hospital between 1 and 13 hours after the onset of symptoms (mean admission time 6.45 hours).
The usual care group was comprised of 7 male and 12 female patients, ages 18–61 (mean age 41.67). They were admitted to the hospital between 1 and 14 hours after the onset of symptoms (mean admission time 6.38 hours). No statistically significant differences in baseline characteristics between the two groups were documented.
Biomedical diagnostic criteria included abdominal pain, anorexia, nausea, vomiting, diarrhea, fatigue, fever, lower-right abdominal tenderness, peritoneal irritation, lower-right abdominal masses, increased white blood cell counts indicating infection or inflammation, and an enlarged appendix as identified by ultrasound. TCM (traditional Chinese medicine) criteria included a diagnosis of qi stagnation/blood stasis or stasis plus heat. A diagnosis of qi stagnation/blood stasis was differentiated by the following symptoms: abdominal distension, nausea and vomiting (with or without fever), red tongue with a white, greasy coating, and a bowstring/tight pulse. A diagnosis of stasis plus heat was differentiated by lower-right abdominal pain, intense rebound pain, muscular tension, fever, dry mouth, constipation, dark urine, red tongue with a yellow or yellow-greasy coating, and a bowstring/slippery/rapid pulse.
In addition to meeting the above diagnostic criteria, patients were required to be between ages 18–65 without any prior appendicitis treatment. Exclusion criteria were comprised of: underlying disease, pregnancy, intention to become pregnant, lactation, allergies to the treatment used in the study, inability to strictly follow medical advice, and cessation of treatment midway through the study.
Patient Care
All patients received usual care, which was comprised of nutritional support, symptomatic relief, semi-solid food, and antibiotic treatment. The antibiotics used in the study were ceftriaxone and tinidazole (intravenous infusions). The ceftriaxone dosage was 2 grams (up to 250 ml with 0.9% saline) and the tinidazole dosage was 0.4 grams. Both antibiotics were administered twice daily. In addition, the patients in the acupuncture and herbs group received herbal medicine and warm needle acupuncture. The herbal formula was comprised of the following herbs:
- Jiu Da Huang 10 g
- Chai Hu 10 g
- Huang Qin 10 g
- Fa Ban Xia 10 g
- Tao Ren 15 g
- Chi Shao 15 g
- Dong Gua Zi 15 g
- Bai Jiang Cao 30 g
- Mu Dan Pi 12 g
- Dan Shen 12 g
- Bran-fried Bai Zhu 12 g
The above formula was administered daily, divided into two doses to be taken morning and evening. Acupuncture was administered at the following acupoints:
- Ashi points
- Zhongwan (CV12)
- Tianshu (ST25)
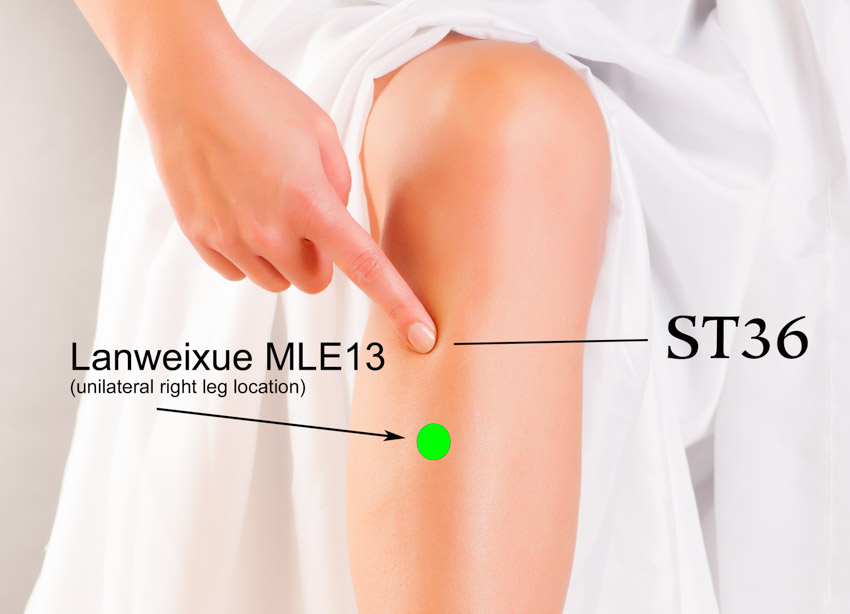
- Zusanli (ST36)
- Lanweixue (appendix point: MLE13)
- Shangjuxu (ST37)
Ashi points were selected on the lower abdomen and 0.3 × 40 mm needles were inserted perpendicularly following standard disinfection. The remaining points were used bilaterally. Following standard disinfection, 0.3 x 40 mm needles were inserted and, after eliciting deqi, pieces of moxa were attached to the handles. The moxa was ignited and replaced at 8-minute intervals and the needles were retained for 40 minutes. One course of each treatment was comprised of 3 days, and a total of 1–3 courses were administered.
The study’s outcome measures included the time taken to regulate bodily temperatures, time taken to resolve abdominal pain, duration of hospital stays, and the total effective rates for each treatment group. Mean time to regulate body temperatures was 1.35 days in the acupuncture and herbs group and 3.61 days in the usual care group. Body temperatures were regulated significantly faster in the acupuncture and herbs group (p<0.05). Mean time to resolve abdominal pain was 3.08 days in the acupuncture and herbs group and 5.96 days in the usual care group. Relief was achieved significantly faster in the acupuncture and herbs group (p<0.05).
Mean hospital stay durations were 4.91 days in the acupuncture and herbs group and 7.19 days in the usual care group. Patients experienced a faster recovery time with acupuncture and herbs (p<0.05). This indicates a potential cost-effectiveness model of care. Although the addition of acupuncture and herbs involves more procedures, this investment in patient care is offset by earlier releases from the hospital.
The total effective rates were calculated for each group. Patients with a complete resolution of symptoms, negative abdominal signs, with normal blood work and ultrasound results, were classified as cured. Patients with significant symptomatic relief but positive abdominal signs and improved blood work and ultrasound results were classified as improved. In patients showing no improvements, the treatment was classified as ineffective. The cured and improved cases in each group were added together to give the total effective rate.
In the acupuncture and herbs group, there were 15 cured, 2 improved, and 1 ineffective case, yielding a total effective rate of 94.44%. In the usual care group, there were 14 cured, 3 improved, and 2 ineffective cases, yielding a total effective rate of 89.47%.
The results of this study indicate that Chinese herbal medicine and warm needle acupuncture are useful adjuncts to standard care in the treatment of acute appendicitis. TCM modalities speed recovery and reduce hospitalization times, thereby reducing costs associated with extended in-patient visits.
The Healthcare Medicine Institute (HealthCMi) offers a continuing education course for licensed acupuncturists on the treatment of chronic appendicitis. Learn more by clicking on the following title of the course: Colitis, Crohn’s Disease, Chronic Appendicitis >
The course is an ebook presentation, which is written material in the PDF format featuring biomedicine, acupuncture, and herbal medicine. The course is presented by HealthCMi author and presenter, Prof. Richard Liao, L.Ac. He has served as professor of herbology and acupuncture theory at the Academy of Chinese Culture & Health Sciences (Oakland, California) and at Five Branches University (Santa Cruz, California). Prof. Liao is currently an active member of the HealthCMi team of authors and presenters.
Reference:
1. He Pengjie (2019) “Clinical observation of oral Chinese medicine combined with warm acupuncture in the treatment of acute, simple appendicitis,” China’s Naturopathy, Vol.27 (17) pp. 48-49.


