Acupuncture provides relief for patients with insomnia. Modern research demonstrates that acupuncture improves sleep quality by regulating central nervous system responses. [1] The investigation covered in this review used scalp acupuncture in conjunction with a sleep medication. Scalp acupuncture is a specialized form of micro-acupuncture, which is commonly utilized by licensed acupuncturists. The combination of drugs plus acupuncture produced superior insomnia relief over drug monotherapy, indicating that an integrative medicine approach to patient care produces greater outcomes.
There were 62 patients in the sample size of this investigation, with an age range of 40–80 years. Randomization of the participants into two groups was performed. The drug observation group was comprised of 12 males and 19 females, mean age 61.3 ±6.3 years. The Pittsburgh Sleep Quality index (PSQI) score was 12.89 ±1.39 prior to treatment. The electroacupuncture group was comprised of 11 males and 20 females, mean age 62.3 ±7.5 years. The PSQI score was 13.01 ±1.30 prior to treatment. There was no significant statistical distinction between the two groups at the outset.
Inclusion criteria were as follows: patients had difficulty in falling asleep or poor sleep quality, and this condition occurred at least 3 times per week, insomnia duration was longer than 1 month, patients developed anxiety due to poor sleep quality, patients presented dissatisfaction with overall sleep, and impairment of patients’ functional status due to sleep dysfunction. All patients met the WHO International Classification of Disease-10 (ICD-10) diagnostic criteria for primary insomnia.
Patients in the drug observation group were administered regular pharmaceutical treatments. Eszopiclone (3 mg) was taken orally at bedtime. This drug is known by its brand name, Lunesta. It is a sedative (hypnotic) that induces relaxation and promotes sleep. Although a non-benzodiazepine prescription medication, eszopiclone may be habit-forming. Treatment lasted for 12 weeks.
In the acupuncture group, patients received scalp acupuncture in addition to eszopiclone. Scalp acupuncture lines were chosen: Middle Line of Forehead (E Zhong Xian, 额中线, MS1) and Lateral Line 1 of Forehead (E Pang Yi Xian, 额旁一线, MS2). Filiform needles of 1.5 cun in length were swiftly inserted into the skin at a 30 degree angle. The tip of the needles reach the epicranial aponeurosis, noted by a decrease in resistance to needling. Then, needles were adjusted to make them more transverse to the skin. In this process, a twisting needle manipulation technique was applied, until the needles reached a depth-length of 1 cun. After this, needles were retained for 20 minutes. The Lateral Line 1 of Forehead lines (bilateral) were connected to an electroacupuncture device using a continuous wave. Scalp acupuncture was administered 5 times per week for 12 weeks.
At HealthCMi, much of our scalp acupuncture investigations reveal excellent results using the scalp system contemporized by Prof. Ming Qing Zhu, L.Ac. Considered one of the great luminaries in the field of scalp acupuncture and the treatment of neurologic conditions, his approach to tonification and attenuation with the chouqi and jingqi techniques has proven itself to be an invaluable tool for helping patients with post-stroke syndrome, post-polio syndrome, and many other disorders. In many ways, the Prof. Zhu system and acupuncture techniques represent some of the most important advances in Chinese medicine in modern history.
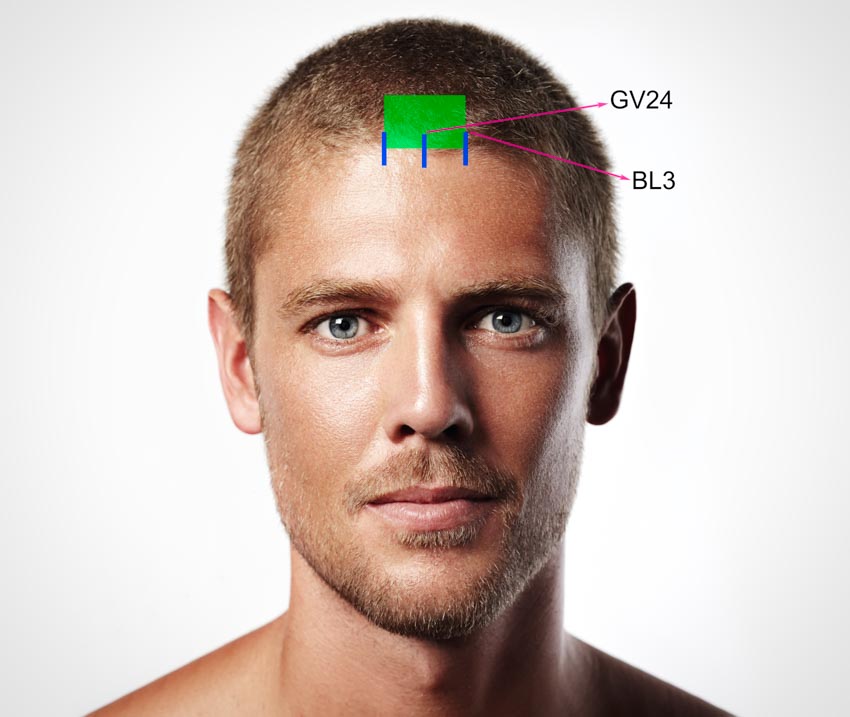
In the research covered in this review, we see a return to the basic international standard of scalp acupuncture system. The scalp acupuncture point selections were Middle Line of Forehead (E Zhong Xian, 额中线, MS1) and Lateral Line 1 of Forehead (E Pang Yi Xian, 额旁一线, MS2). Both MS1 and MS2 overlap with the Prof. Zhu scalp system’s head-face zone. The head-face zone and the scalp acupuncture lines chosen for this investigation center around acupuncture points GV24 and BL3.
BL3 is directly superior to BL2, which is superior to the inner canthus in the depression that is palpable in the medial aspect of the eyebrow. BL3 is located above this acupoint, 0.5 cun within the anterior hairline. Lateral Line 1 of Forehead (E Pang Yi Xian, MS2) is a 1 cun line starting at BL3 and extending anteriorly toward the forehead, bilaterally. Middle Line of Forehead (E Zhong Xian, MS1) extends 1 cun anteriorly from GV24 toward yintang.
After treatment, the acupuncture group experienced a more significant decrease in PSQI scores, dropping from an average of 12.89 ±1.39 to 3.63 ±1.13. By contrast, the figure for the drug observation group presented a smaller change from 13.01 ±1.30 to 6.23 ±1.06. In addition, the acupuncture group showed a higher patient satisfaction rate of 96.8%, which is 10.2% higher than that of the drug observation group. The researchers concluded that for patients with primary insomnia, scalp acupuncture with electroacupuncture combined with conventional drug therapy markedly improves sleep and is superior to drug monotherapy.
Reference
[1] Liu Kun, Study on the effect of scalp acupuncture combined with electric acupuncture on primary insomnia, China Journal of Modern Drug Application, Nov 2020, Vol. 14, No. 22.


