Acupuncture is an effective treatment for the relief of insomnia. Two independent research teams from the Heilongjiang University of Chinese Medicine found acupuncture over 90% effective for the treatment of insomnia. In addition, Li et al. found an important biochemical basis for the efficaciousness of acupuncture in the treatment of insomnia. 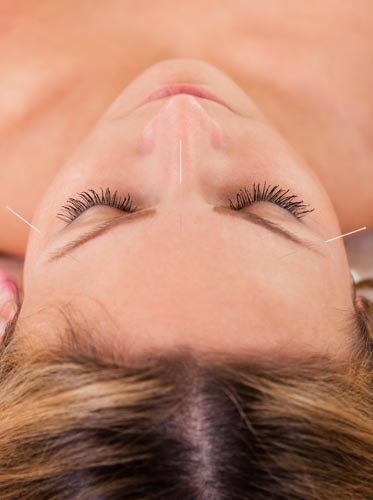
Li et al. conducted an investigation and determined that acupuncture increases biochemical concentrations that benefit sleep. Acupuncture increases the concentration of gama-aminobutyric acid (GABA) in cerebrospinal fluid and increases bodily serotonin (5-HT) levels. Serotonin is involved in the regulation of many bodily functions including appetite, cognitive function, mood, and sleep. GABA is a neurotransmitter that produces inhibitory responses to postsynaptic neurons in the adult brain.
In one of two recent investigations at the Heilongjiang University of Chinese Medicine, researchers tested two acupuncture insomnia treatment protocols. One protocol, called Tiao Shen, achieved a 93.3% total effective rate for the treatment of insomnia. The second treatment protocol, a standardized form of body style acupuncture, achieved a 73.3% total effective rate. Sixty patients were randomized into two equal groups in a semi-protocolized trial.
Group one received the Tiao Shen protocol. Primary body style acupuncture points included:
DU24, Shenting
HT7, Shenmen
ST36, Zusanli
SP6, Sanyinjiao
DU16, Fengfu
GB13, Benshen
Yintang
Sishencong
Anmian
Supplementary acupuncture points were added based on differential diagnostics -
Spleen and heart deficiency: add BL15 (Xinshu), BL20 (Pishu)
Heart and kidney deficiency: add HT8 (Shaofu), KD3 (Taixi)
Liver disharmony: add LV3 (Taichong), LI4 (Hegu)
Heart deficiency: add BL15 (Xinshu), BL19 (Danshu)
Excess phlegm: add PC6 (Neiguan), ST40 (Fenglong)
Deqi was elicited at the body style acupuncture points with mild reinforcing and reducing techniques. Total needle retention time was 45 minutes per acupuncture session. The Tiao Shen protocol involved the addition of auricular acupuncture points including subcortex, shenmen, and others. The points were stimulated with vaccaria seeds covered with zinc oxide tape. Patients were advised to stimulate the auricular points 3 to 5 minutes per day. 
Group two received acupuncture at body style acupuncture points only. The primary acupuncture points were:
HT7, Shenmen
HT3, Shaohai
BL62, Shenmai
Yintang
Sishencong
Anmian
The same manual acupuncture techniques and treatment duration applied to group two as in group one. The clinical success rate for improving sleep quality and duration differed significantly between group one and two. Group one achieved a 93.3% total effective rate and group two achieved a 73.3% total effective rate. The results suggest that the addition of auricular acupuncture enhances the clinical efficacy of body style acupuncture.
Another research team at the Heilongjiang University of Chinese Medicine investigated the efficacy of Sun's abdominal acupuncture protocol for the treatment of insomnia. The data demonstrates that combining Sun’s abdominal acupuncture point prescription with standard acupuncture points improves the clinical success rate for the treatment of insomnia. The Sun abdominal acupuncture protocol achieved a 96.67% total effective rate. This was compared with a conventional acupuncture protocol that achieved a 76.67% total effective rate.
The Sun acupuncture point protocol consists of three main abdominal acupoints. The first point is a half inch below the xiphoid process. The other two points are each one inch lateral to this point on both the left and right sides. According to the Sun system, this acupuncture point combination is indicated for the treatment of anxiety, depression, insomnia, forgetfulness, obsessive-compulsive disorder, epilepsy, and dream disturbed sleep.
Patients receiving Sun’s abdominal acupuncture also received acupuncture at the following acupuncture points:
Yintang
Sishenchong
Anmian
HT7, Shenmen
HT3, Shaohai
BL62, Shenmai
Electroacupuncture was applied to Anmian and the lateral Sun abdominal acupoints. Supplementary acupuncture points were added based on differential diagnostics -
For heart and spleen deficiency add BL15 (Xinshu) and BL20 (Pishu).
For phlegm fire add ST40 (Fenglong) and ST44 (Neiting).
For deficiency of the heart, gallbladder, and qi add BL15 (Xinshu) and BL19 (Danshu).
For deficiency of the heart and kidneys add BL15 (Xinshu) and BL23 (Shenshu).
For disharmony of the spleen and stomach add SP4 (Gongsun) and ST36 (Zusanli).
The Sun acupuncture protocol improved many aspects of the Pittsburgh Sleep Quality Index (PSQI). The 96.67% total effective rate demonstrates that the Sun acupuncture protocol is effective for the treatment of insomnia. The Wang et al. research, using the Tiao Shen protocol that achieved a 93.3% total effective rate, also shows significant positive patient outcomes for patients with insomnia.
Both acupuncture and Chinese herbal medicine have a long and established history of treatment protocols for the relief of insomnia. This includes everything from ancient writings to modern research. At the Healthcare Medicine Institute, we offer several courses on the treatment of sleep disorders including the acupuncture continuing education course entitled Pain, Headaches, Insomnia, and Fear. Translated by Prof. Richard Liao, L.Ac., this course features several important herbal medicine treatments for the relief of insomnia. The course features the writings of Dr. Di, an important early 20th century Chinese medicine physician whose treatment strategies are venerated to this day.
References:
Wang H., Meng X.H., Zou W. (2014). Curative Effect of Acupuncture Therapy of Regulating Mentality Combined with Auricular Point in the Treatment of Insomnia. Journal of Clinical Acupuncture and Moxibustion. 30(7).
Li YH, Zhang LT. (2009). Acupuncture therapy in treating athletic insomnia and its effects on the levels of 5-HT and NGF. Zhe Jiang Journal of TCM. 44(6): 402.
Sun YZ & Yu T. (2014). Clinical Research on the First Area of Sun’s Abdominal Acupuncture Treatment for Insomnia. Journal of Clinical Acupuncture and Moxibustion. 30(12).
Gottesmann, Claude. "GABA mechanisms and sleep." Neuroscience 111, no. 2 (2002): 231-239.


