A new controlled study finds acupuncture effective for improving balance in stroke patients. Researchers from Taipei Medical University (Shuang Ho Hospital, Taiwan) and three additional hospitals compared a control group with an acupuncture group. The acupuncture group demonstrated clinically superior clinical outcomes for hemiplegic stroke patients. 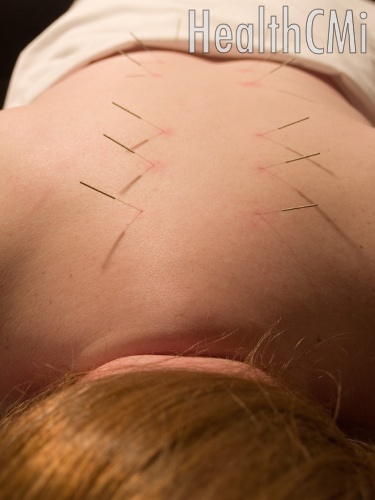
The study was conducted at the medical university hospital ward. A total of 66 patients were randomly assigned to each group for a total of 132 participants. The results show that acupuncture improves static balance when added to the rehabilitation phase of treatment for hemiplegic stroke patients with a low Brunnstrom (Br) stage. The Br stages, developed by a Swedish physical therapist, measures levels of motor activity and account for flaccidity, synergy, voluntary movements, spasticity, complex movements, individual joint movements and the restoration of normal function.
The study design reflects common practice for licensed acupuncturists. Physiotherapy was combined with acupuncture for the acupuncture treatment group and physiotherapy was administered as a standalone treatment modality for the control group. Postural assessment scales were measured for both static and dynamic balance values. Definitive positive clinical results demonstrate that acupuncture causes a significant increase in static balance measures for hemiplegic stroke patients when combined with physiotherapy.
Large Scale Investigation
This recent acupuncture continuing education study confirms additional investigations demonstrating that acupuncture is an effective medical modality for the treatment and prevention of strokes. One recent study finds acupuncture effective for reducing the risk of stroke for patients with traumatic brain injuries. An investigation of approximately 30,000 patients reveals that patients receiving acupuncture have a “lower probability of stroke than those without acupuncture treatment during the follow-up period.” The study “showed significantly decreased risk of new-onset stroke events for patients with TBI (Traumatic Brain Injury) who received acupuncture treatment. The present study is the first to report that acupuncture treatment was associated with reduced stroke risk for patients with TBI.”
Investigators at Heilongjiang University of TCM note that clinical outcomes are improved for stroke patients when scalp acupuncture is combined with body style acupuncture and/or physical therapy. Several studies were examined in this meta-analysis. In one study under the auspices of Zhen Yongqiang, body style acupuncture was 75% effective and scalp acupuncture 76% was effective. However, combining the modalities increased the total effective rate to 87%. Zhuang Jie’s study measured a combination of scalp acupuncture and physical rehabilitation. Scalp acupuncture as a standalone procedure achieved a 77% total effective rate but the combination of scalp acupuncture with physical rehabilitation increased the total effective rate to 97%. An additional study examined by the Heilongjiang University of TCM researchers measured significant improvements in patient outcomes for stroke patients when acupuncture is combined with the herbal formula Bu Yang Huang Wu Tang (Tonifying Yang Decoction for Recuperation). The total effective rate using acupuncture combined with the herbal formula was 96%.
Another investigative team discovered that acupuncture is effective for the treatment of post-stroke hand movements and walking dysfunction. Researchers investigated the use of acupuncture points TB3 (Zhongzhu) and TB5 (Waiguan). A randomized patient sample was divided into a treatment group and a control group. Both groups received physical therapy, occupational therapy and other conventional rehabilitative procedures. Both groups were evaluated for changes in walking, hand function and activities of daily living. The group receiving acupuncture at TB3 and TB5 showed significant improvements over the control group. The acupuncture group demonstrated superior hand function, greater walking ability and enhanced activities of daily living. The researchers conclude that the combination of acupuncture with routine post-stroke recovery procedures produces significantly improved patient outcomes.
MRI Study
The evidence for acupuncture’s ability to enhance stroke recovery is supported by objective data. A groundbreaking study proves that acupuncture increases brain activity and functionality for stroke patients. The researchers also demonstrated that sham acupuncture did not increase brain activity and functionality.
Using fMRI and microPET imaging techniques, the researchers were able “to measure the glucose metabolic level in the brain which is an important index of brain function.” Acupuncture points Bai Hui (GV20) and Shui Gou (GV26) were applied to patients in the verum acupuncture group. The results were repeatable and measurable. Acupuncture was proven to increase brain activity in the acute stage of an ischemic stroke using the brain glucose metabolic level as a quantitative index. The sham acupuncture group and a control group did not demonstrate increases in brain activity and functionality.
Shoulder Pain
Another investigation proves acupuncture effective for the treatment of shoulder pain following a stroke. Approximately 70% of stroke patients develop significant shoulder pain. The researchers conducted a meta-analysis of 453 randomized controlled studies of acupuncture for the treatment of shoulder pain after a stroke. Based on the evidence, the researchers conclude that “acupuncture is an effective treatment for shoulder pain after (a) stroke.”
Another acupuncture continuing education study finds acupuncture effective in reducing infarct size after ischemia/reperfusion injuries (CIRI). The researchers note that acupuncture “significantly reduced infarct size and improved neurologic function.” They add that acupuncture exerts “neuroprotective actions.” 
Microscopic evaluation, fMRI, hematoxylin-eosin staining, quantitative real-time polymerase chain reaction evaluation, immunofluorescence analysis, immunohistochemical analysis and western blot analysis confirm the effectiveness of acupuncture for the reduction of infarct sizes. Application of acupuncture points GV20 and ST36 reduced infiltration of inflammatory cells, downregulated expression of proinflammatory enzyme MMP2, reduced expression of water channel proteins AQP4 and AQP9, reduced brain ischemia and decreased brain edema due to inflammation. Neurologic functions improved including balance and reflexes. The researchers conclude, “acupuncture and electroacupuncture are effective treatments for brain tissue injury and neurological deficits following CIRI in rats. Therefore, this study adds to the growing arsenal of research supporting the view that acupuncture and electroacupuncture, which are derived from Traditional Chinese Medicine, can serve as complementary and alternative treatments to supplement the conventional management of ischemic stroke.”
References:
Huang, Shih-Wei, Wei-Te Wang, Tsung-Hsien Yang, Tsan-Hon Liou, Guan-Yu Chen, and Li-Fong Lin. "The Balance Effect of Acupuncture Therapy Among Stroke Patients." The Journal of Alternative and Complementary Medicine.
Shih, Chun-Chuan, Yi-Ting Hsu, Hwang-Huei Wang, Ta-Liang Chen, Chin-Chuan Tsai, Hsin-Long Lane, Chun-Chieh Yeh et al. "Decreased Risk of Stroke in Patients with Traumatic Brain Injury Receiving Acupuncture Treatment: A Population-Based Retrospective Cohort Study." PLOS ONE 9, no. 2 (2014): e89208.
Chen, Li and Zhongren Sun. “Research on Treating Stroke by Head Acupuncture Therapy.” Clinical Journal of Chinese Medicine 6.1 (2014).
Cheng XK, Wang ZM, Sun L, Li YH. [Post-stroke hand dysfunction treated with acupuncture at Zhongzhu (TE 3) and Waiguan (TE 5)]. Zhongguo Zhen Jiu. 2011 Feb;31(2):117-20.
Using MicroPET Imaging in Quantitative Verification of Acupuncture Effect in Ischemia Stroke Treatment, Xiaoyan Shen1, Hongtu Tang2, Jia Li2, Ting Xiang2, Huafeng Liu1 & Weichuan.
Jung Ah Lee, Si-Woon Park, Pil Woo Hwang, Sung Min Lim, Sejeong Kook, Kyung In Choi, and Kyoung Sook Kang. The Journal of Alternative and Complementary Medicine. September 2012, 18(9): 818-823. doi:10.1089/acm.2011.0457.
Hong Xu, Yamin Zhang, Hua Sun, Suhui Chen, Fuming Wang
Research Article | published 14 May 2014 | PLOS ONE
10.1371/journal.pone.0097488.


