Acupuncture increases the effectiveness of paroxetine (Paxil, Aropax) for the treatment of depression. Researchers from the Beijing University of Chinese Medicine conducted a controlled investigation and found that both manual and electroacupuncture significantly increase the total effective rate of paroxetine.  Prior research by Qu et al. finds acupuncture effective for enhancing the effects of paroxetine for the treatment of major depression. The Beijing University of Chinese Medicine researchers build on these findings by demonstrating that acupuncture enhances the effects of paroxetine for the treatment of mild and moderate level depression.
Prior research by Qu et al. finds acupuncture effective for enhancing the effects of paroxetine for the treatment of major depression. The Beijing University of Chinese Medicine researchers build on these findings by demonstrating that acupuncture enhances the effects of paroxetine for the treatment of mild and moderate level depression.
The researchers discovered a great advantage to adding acupuncture therapy to paroxetine therapy. Not only did acupuncture enhance antidepressant actions, it also significantly reduced adverse effects caused by the medication. Acupuncture reduced levels of paroxetine induced urinary disorders, sexual dysfunction, headaches, dizziness, constipation, and insomnia.
Patients with mild to moderate depression were selected according to inclusion and exclusion criteria from the Peking University Sixth Hospital, First Affiliated Hospital of Nanjing University of Traditional Chinese Medicine, Southern Medical University, and the Baotou City Mental Health Center. A total of 72 patients were randomly divided into three groups. One group received electroacupuncture and paroxetine. Another group received manual acupuncture and paroxetine. A third control group received only paroxetine.
The electroacupuncture plus paroxetine group had an effective rate of 95%. The manual acupuncture plus paroxetine group had an 81.48% effective rate. The paroxetine only group had a 50% effective rate.
Drug Treatment
All three groups received treatment for 6 weeks and the patients were evaluated 4 weeks after completion of the treatment sessions. Paroxetine was administered at a dose of 10 mg per day for the first two days. Next, the dosage was increased to 20 mg per day. The paroxetine was taken orally after breakfast for 6 weeks.
Acupuncture Therapy
Manual acupuncture was applied at a rate of once every other day. 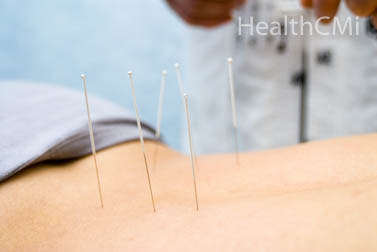 Needle manipulation techniques were applied for 5 - 10 seconds at the 15 minute mark and prior to removing the needles at the end of the 30 minute needle retention period. Primary acupuncture points were:
Needle manipulation techniques were applied for 5 - 10 seconds at the 15 minute mark and prior to removing the needles at the end of the 30 minute needle retention period. Primary acupuncture points were:
- GV20, Bai Hui
- Yintang, extra point
A total of 1 - 2 secondary acupoints were chosen based on signs and symptoms per each patient and included:
- GV16, Fengfu
- GB20, Fengchi
- DU14, Dazhui
- PC6, Neiguan
- SP6, Sanyinjiao
The electroacupuncture group received 2 - 15 Hz electricity to patient tolerance levels. Acupuncture was applied once every other day and the treatment sessions were 30 minutes in length. The main acupoints were:
- DU20, Baihui
- Yintang, extra pont
- GB20, Fengchi
Evaluation standards were largely based on the Hamilton Depression Scale. A reduced rate of depression above 75% was defined as clinical mitigation, above 50% was termed significant effectiveness, and above 25% was termed improvement. Less than or equal to 25% means ineffective. The total effective rate was calculated based a greater than 25% improvement on the Hamilton Depression Scale.
The researchers concluded that acupuncture enhances the therapeutic effects of paroxetine for patients with mild to moderate depression. Electroacupuncture was more effective than manual acupuncture. In addition, acupuncture reduced iatrogenic adverse effects caused by the medication including significant reductions of fatigue, headaches, dizziness, palpitations, tremors, sweating, dry mouth, constipation, urinary disorders, sexual dysfunction, and sleep disorders. The findings suggest that an integrative medicine approach delivers significantly greater positive patient outcomes over an isolated drug therapy regimen of care.
References:
Kessler RC.Epidemiology of women and depression [J].Affect Disord,2003,74(1):5-13.
Wang, S. H., Wang, Y. Z., Ma, X. H., Guo, Z., Yang, X. J., Zhang, W. Y., Guo, T. W. and Tu, Y. (2014). Study on alleviating side effect of paroxetine and improving quality of life using acupuncture in treatment of mild or moderate depression. Chinese Journal of Behavioral Medicine and Brain Science. 23 (3).
Wang, Tianjun, Lingling Wang, Wenjian Tao, and Li Chen. "Acupuncture combined with an antidepressant for patients with depression in hospital: a pragmatic randomised controlled trial." Acupuncture in Medicine (2014): acupmed-2013.
Qu SS, Huang Y, Zhang ZJ, et al. A 6-week randomized controlled trial with 4-week follow-up of acupuncture combined with paroxetine in patients with major depressive disorder. J Psychiat Res 2013;47:726–32. 13 Zhang ZJ, Ng R, Man SC, et al. Dense cranial.


