Acupuncture alleviates depression and insomnia. Research published in the Shanghai Journal of Acupuncture and Moxibustion (Ye et al.) finds acupuncture 90% effective in improving total sleep duration and sleep quality for patients with depression. Alleviation of insomnia directly correlated to improvements in the mental and physical health of study participants. Acupuncture treatments lowered relapse rates and produced similar clinical results as antidepressants. Notably, acupuncture did not produce any adverse effects. 
Two groups were compared. Group one received acupuncture and group two received oral tablets of mirtazapine, an antidepressant drug. Acupuncture therapy achieved a 90% total effective rate and mirtazapine therapy achieved a 92.5% total effective rate. Common mirtazapine adverse effects include dizziness, drowsiness, vision changes, weight gain, increased appetite, and constipation. No adverse effects occurred in study participants receiving acupuncture.
Insomnia due to depression, termed depressive insomnia in Traditional Chinese Medicine (TCM), is characterized by difficulty falling asleep, dream disturbed sleep, generalized insomnia, and severe emotional fluctuations. Additional symptoms include major depression, loss of appetite, exhaustion, chest tightness, manic states, pain of the hypochondriac region, and excessive pessimism.
Hamilton Depression Rating Scale (HAM-D) results measured demonstrative improvements in both the acupuncture and drug therapy patients. The acupuncture group demonstrated a 9.7% HAM-D score improvement within one month of treatment. The HAM-D score improved by 36.2% within three months. The drug group demonstrated a HAM-D score improvement of 15.9% within one month and 32.5% within three months.
The total effective rate was determined by adding all patients with 30% – 100% clinical improvements. The acupuncture group achieved a 90% total effective rate. The drug therapy group achieved a 92.5% total effective rate.
The drug therapy group received 20 mg of mirtazapine tablets orally at a rate of once per day for three months. The acupuncture group received acupuncture treatment sessions every other day. An exception was made for extreme cases of depressive insomnia; these patients received acupuncture at a rate of once per day. Treatments were applied over a three month period.
The patients received a semi-protocolized acupuncture point prescription comprised of a set of primary acupuncture points for all patients and a set of secondary acupuncture points for specific differential diagnostic conditions. The primary acupoints were
- Shenmen (HT7)
- Sanyinjiao (SP6)
- Yintang (extra)
Secondary acupoints were administered when one of two of the following conditions were diagnosed. For patients with the TCM diagnosis of liver qi stagnation, Taichong (LV3) and Yanglingquan (GB34) were added. For patients with heart and spleen related disorders, Zusanli (ST36) and Jianshi (PC5) were added. Manual acupuncture stimulation was applied to the needles to elicit deqi followed by a thirty minute needle retention time. During the needle retention period, manual needle stimulation was applied every ten minutes using lifting and thrusting techniques for sedation and tonification. 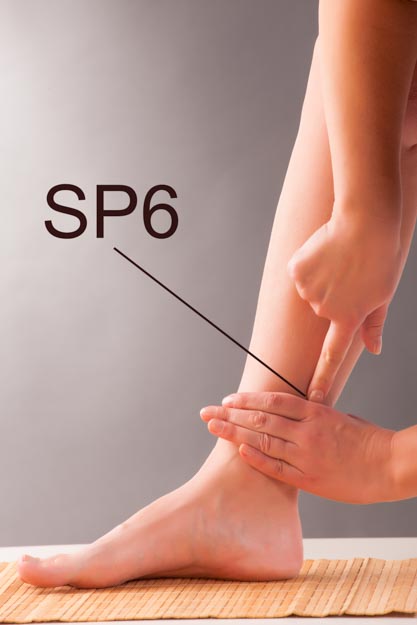
The researchers conclude that acupuncture significantly improves sleep time and sleep quality while improving the overall mental and physical health of patients. No adverse effects occurred. Moreover, acupuncture reduced the relapse rate for depressive insomnia.
Lin et al. had similar findings. Their research finds acupuncture points Lieque (LU7) and Zhaohai (KD6) potent clinical tools in the fight against generalized anxiety disorder (GAD). Lin et al. note that “a number of Meta analysis and system evaluations point out that acupuncture treatment has more advantages than drugs in the treatment of anxiety disorders….” Lin et al. add that acupuncture has a fast effective action, high compliance to the therapeutic regimen, and a relatively minimal risk of side effects compared with drug therapy.
The research of Wang et al. confirms the aforementioned studies. Wang et al. conclude that acupuncture benefits sleep and reduces insomnia in a single-blinded, randomized, placebo-controlled investigation comparing acupuncture with sham acupuncture and estazolam, a benzodiazepine medication. True (verum) acupuncture produced significantly superior patient outcomes for insomnia patients including improvements in sleep quality and total sleep time. Primary acupuncture points used in the study were
- Shenting (DU24)
- Sishencong (EX-HN1)
- Baihui (DU20)
- Shenmen (HT7)
- Sanyinjiao (SP6)
Acupuncture restored nighttime sleep and improved daytime energetics. Patients in the estazolam medication group experienced adverse effects including daytime drowsiness that typically ceased by midday. The researchers note, “The trial implied that verum acupuncture was superior in improving sleep quality and daytime functioning of primary insomnia compared with estazolam and sham acupuncture.” The researchers note that true acupuncture increased total sleep time and “improved sleep quality (SQ) and vitality (VT), decreased daytime dysfunction (DD) and sleepiness (ESS score).”
References:
Ye GC & Yan H. (2014). Therapeutic Observation of Acupuncture for Depressive Insomnia. Shanghai Journal of Acupuncture and Moxibustion. 55(6).
Observation on the mechanism of acupuncture treatment for generalized anxiety disorder using Lieque (LU7), Zhaohai (KI6) as the main acupoints. Lin, Chuhua; Zhao, Xiaoyan; Liu, Xing; Fu, Wenbin. Bioinformatics and Biomedicine (BIBM), 2013 IEEE International Conference on. 18-21, 12-2-13.
Lin-Peng Wang, Guo, Jing, Cun-Zhi Liu, Jie Zhang, Gui-Ling Wang, Jing-Hong Yi, Jin-Lian Cheng, and R. Musil. "Efficacy of acupuncture for primary insomnia: a randomized controlled clinical trial." Deutsche Zeitschrift für Akupunktur 57, no. 4 (2014): 31-32.


