Acupuncture is effective for the treatment of facial paralysis and improves patient outcomes for patients taking medications.
Hospital researchers find acupuncture effective for the treatment of facial paralysis. Across multiple hospital investigations, researchers document effective acupuncture protocols that yield significant positive patient outcomes for facial paralysis patients. In addition, acupuncture, infrared therapy, and moxibustion demonstrate the ability to significantly improve positive patient outcome rates for patients taking pharmaceutical medications.
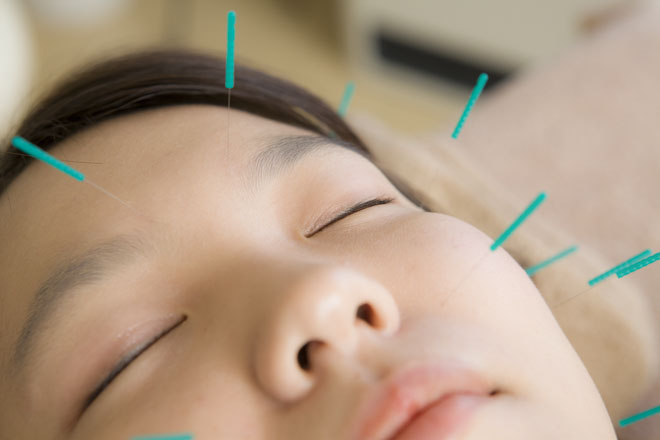
 Facial Acupuncture Needling
Facial Acupuncture Needling
Acupuncture and infrared heat therapy are effective for the treatment of facial paralysis. Researchers from the Third People’s Hospital in Chongqing determined that combining acupuncture and infrared heat therapy with conventional facial paralysis medications improves the rate of positive patient outcomes for the the treatment of this condition. Facial paralysis is a disorder in which the facial muscles are dysfunctional, causing immobility, and it may occur in any age demographic. In the Third People’s Hospital investigation, facial paralysis patients who received supplementary infrared heat therapy and acupuncture reported a 91.67% total treatment effective rate while those in the control group reported a 60.42% total treatment effective rate. The addition of acupuncture and infrared therapy increased the effectiveness by 31.25%.
The study involved 96 patients with facial paralysis. Onset was within 6 days of treatment. Of the 96 patients, there were 46 males and 50 females. Patient ages ranged from 46 to 65 years old. The patients were randomly divided into 2 groups: the treatment group and the control group with 48 patients in each group. The control group was given conventional facial paralysis medications: vitamins, hormones, brain glycosides, carnosine and antiviral drugs. The treatment group underwent acupuncture therapy and infrared heat therapy in addition to receiving the same conventional medications as the control group. The total treatment duration was 2 weeks.
For acupuncture, the principles for the treatment of facial paralysis focused on restoring nerve function via improving local blood circulation, eliminating edema, and reducing facial nerve inflammation. The selection of acupoints for facial paralysis treatment largely involves the Yangming and Taiyang meridians. The acupoints include: Zusanli, Hegu, Fengchi, Yifeng, Taiyang, Jiache, Dicang, Zanzhu, and Xiaguan. The Zusanli and Hegu acupoints improve qi and blood circulation and eliminate excess wind (feng). The Fengchi, Yifeng and Taiyang acupoints eliminate wind (feng) and pernicious influences (Xie). The Jiache, Dicang, Zanzhu and Xiaguan acupoints are selected based on the symptoms presented by the individual patient.
Infrared heat therapy utilizes the red spectrum of visible light, which has photochemical effects including: activating catalase in cell mitochondria, increasing glycogen concentration, strengthening cell metabolism, improving adenosine triphosphate decomposition, and protein generation. These processes culminate in accelerated cell synthesis and regeneration, improved local blood microcirculation to the skin and nerves in the affected area, as well as improved metabolism and overall immunity. The net effect on the afflicted facial region is the reduction of nerve tissue inflammation therapy alleviating paralysis.
The primary acupoints selected for the treatment group were:
- Jiache (ST6)
- Xiaguan (ST7)
- Dicang (ST4)
- Yifeng (SJ7)
- Taiyang (EX)
- Zanzhu (BL2)
- Hegu (LI4)
- Fengchi (GB20)
- Zuli
The secondary acupoints selected were:
- Yangbai (GB14)
- Yingxiang (LI20)
- Renzhong (DU26)
- Sibai (ST2)
- Chengjiang (REN24)
Standard acupuncture was administered on these acupoints once daily for 14 consecutive days. Infrared therapy was administered using the Carnation33 high power infrared light therapy device with a 640 nm wavelength (+/- 10 nm). The unit was manufactured by the Shenzhen Universal Gate Science and Technology Co. The affected site of paralysis received infrared heat from a distance of 30 to 35 cm and skin surface temperature was maintained at 40 degrees Celsius, or the highest temperature within the patient’s tolerance zone. The infrared heat therapy therapy was conducted for 20 minutes at a time, 2 times daily, for 14 consecutive days. The conventional facial paralysis medications were as follows:
- Dexamethasone (10–15g). Intravenously injected, once daily, for 10 consecutive days.
- Vitamin B12 (0.5 mg), Vitamin B1 (100 mg). Administered through muscle injection, once daily, continuously for 14 consecutive days.
- Brain glycoside injection fluid (3 ml). Administered through muscle injection, 2 times daily, for 14 consecutive days.
- In cases of viral infections, the patient was given acyclovir tablets (0.4 g), taken orally 3 times daily, for 10 consecutive days.
Treatment efficacy was evaluated and categorized into 4 tiers:
- Recovery: Symptoms and pathological physical signs are not observed. Facial muscle function is restored. Facial appearance is symmetrical.
- Significantly effective: Significant improvement in symptoms and physical signs. Facial muscle function is significantly restored. Facial appearance is largely symmetrical.
- Effective: Improvement in symptoms and physical signs.
- Ineffective: No improvement in symptoms and physical signs.
The treatment group achieved a 91.67% total treatment effective rate; the control group achieved a 60.42% total treatment effective rate. Based on the clinical results of this study, the researchers conclude that acupuncture and infrared heat therapy accelerate facial paralysis recovery and significantly raise the treatment efficacy rate.
Other related research supports the hypothesis that acupuncture is effective for alleviating or eliminating facial paralysis. Researchers from the Shenzhen Chinese Medicine Hospital determined that acupuncture effectively targets the liver stagnation class of facial paralysis cases. They noted that acupuncture, combined with TCM (Traditional Chinese Medicine) intervention, improves positive patient outcomes. Facial paralysis due to liver stagnation often manifests as peripheral facial paralysis. Peripheral facial paralysis is a common disorder of the facial muscles wherein patients present with unilateral, uncontrollable ptosis or drooping of the corner of the mouth. This is termed as Kou Jiao Wai Xie in the TCM lexicon. In many cases, patients experience psychological complications including depression, anxiety and somatization symptoms (Shi and Zhang, 2004).
In TCM, the liver’s main function is to dredge the channels, remove bodily waste, and regulate qi. It is an indispensable organ in regulating qi and blood in the body. Stagnation of the liver causes the facial tendons and meridians (Jin Mai) to receive insufficient qi and blood supply. This may trigger or worsen facial paralysis.
Treatment for this particular type of facial paralysis typically focuses on treating the paralysis directly and keeping the patient in a healthy psychological state. By alleviating depression and anxiety, and reinforcing a positive psychological state, qi and blood circulation is improved thereby facilitating improved patient recovery rates. Procedures in TCM intervention include acupoint massage, psychological counseling, and health education. The Shenzhen Chinese Medicine Hospital study reported that facial paralysis patients experienced a total treatment effective rate of 87.72% with acupuncture and TCM intervention modalities.
57 patients with liver stagnation type peripheral facial paralysis were included in this study. They received standard acupuncture treatment, acupoint massage, psychological counseling and health education in a 4 week long treatment course. Primary acupoints for the acupuncture therapy were the following:
- Zanzhu (BL2)
- Yangbai (GB14)
- Taiyang (EX)
- Yuyao (EX)
- Sibai (ST2)
- Yifeng (SJ17)
- Qianzheng (EX)
- Yingxiang (LI20)
- Dicang (ST4)
- Jiache (ST6)
- Hegu (LI4)
- Taichong (LIV3)
- Yanglingquan (GB34)
- Zulinqi (GB41)
Additional acupoints were selected on a symptomatic basis:
- Chengqi (ST1), Jingming (BL1). For teary eyes due to the wind (feng) element.
- Shuigou (DU26). For deviated philtrum.
- Chengjiang (REN24). For deviated lip cheek groove.
- Jiachengjiang (EX). For severely deviated mouth.
- Lianquan (REN23). For numb tongue and loss of taste.
- Wangu (SI4). For pain at the back of ears and mastoid.
Within 7 days of facial paralysis onset (acute phase), the following rules were observed. Electroacupuncture was not administered. Facial acupoints were inserted carefully to a shallow depth, without any twisting, pushing or pulling techniques. The attenuation (Xie) technique was applied for the Hegu and Taichong acupoints. The mild reinforcement and attenuation (Ping Bu Ping Xie) technique was applied for the Yanglingquan and Zulinqi acupoints. For the above acupoints, a needle retention time of 20 minutes was observed. Acupuncture sessions were conducted once daily.
When patients entered the chronic and recovery phase (7 days after the onset of facial paralysis), the following rules were observed. Acupuncture was administered from Dicang through Jiache, and Yangbai through Yuyao. Other acupoints were treated as per the rules for the acute phase. After each acupuncture session, the following acupoints were massaged on the affected side:
- Yangbai (GB14)
- Taiyang (EX)
- Xiaguan (ST7)
- Quanliao (SI18)
- Dicang (ST4)
- Jiache (ST6)
Firstly, the patient rested in a seated or supine position. The practitioner held the patient’s head with one hand and applied the Yi Zhi Chan Tui massage technique to the above acupoints with the other hand. Each acupoint was massaged for 5 minutes continuously. Patients received the acupuncture and acupoint massage therapy once daily for 6 consecutive days, followed by a 1 day break. The therapy was conducted for a total of 4 weeks.
In addition to administering acupuncture and acupoint massage, treatment included psychological counseling. This involved helping patients to recall positive memories, sharing successful recovery cases, and facilitating intellectual games and decision assignments. These activities minimized depression and anxiety while reinforcing self-confidence. Patients were advised to listen to soothing and melodic music to relieve depression and anxiety. They were also encouraged to find and indulge in interests in their own time including reading, chess, singing, dancing, etc.
The health education treatment module mainly comprised 3 parts: facial care, food consumption, lifestyle care. For facial care, patients were instructed to use warm water to wash their face and brush their teeth. Additionally, they were taught facial muscle exercises including frowning, whistling, and inflating the cheek (to be performed 2 to 3 times per day).
For food consumption, patients were instructed to consume easily digestible light foods such as fish and lean meats. Rice, noodles and roughage were also included to ensure a sufficient supply of energy. Patients were reminded to avoid sour, hard, dry, coarse, spicy, fried and spicy-hot foods. For lifestyle care, patients were advised to get sufficient rest and exercise and to avoid exposure to cold and dampness (including rain) by wearing protective glasses, masks, or other forms of protection.
The total treatment effective rate was evaluated based on the TCM Syndrome Diagnosis and Treatment Efficacy Standard and the House-Brackmann Classification of Facial Function. Among the 57 patients, 13 patients recovered completely, 12 patients had significantly effective results, 25 patients had modest improvements, and 7 patients had no improvements. The total treatment effective rate was 87.72%. The researchers conclude that acupuncture with TCM intervention therapy is an effective protocol for the treatment of liver stagnation type facial paralysis.
In another study on facial paralysis and acupuncture, researchers from hospitals in Changsha and Yueyang determined that acupuncture and moxibustion produce positive patient outcomes in eliminating or alleviating facial paralysis. Acupuncture and moxibustion have proven efficacy in treating facial paralysis (Li et al., 2005). It is interesting to note, though, that acupuncture and moxibustion therapies are often only conducted during the recovery phase of facial paralysis.
The Changsha and Yueyang study showed that facial paralysis patients who received acupuncture and moxibustion treatment had a total treatment effective rate of 74.9%. The control group had a total treatment effective rate of 51.8%. More specifically, the acupuncture and moxibustion treatment group saw a 30.1% complete recovery rate and a 44.8% significantly effective treatment rate. On the other hand, the control group saw a 17.4% complete recovery rate and 34.4% significantly effective treatment rate. For this study, 624 patients with facial paralysis were randomly divided into two groups: treatment group, control group. Each group was comprised of 312 patients. Selected primary acupoints for the treatment group were:
- Dicang (ST4)
- Jiache (ST6)
- Hegu (both sides) (LI4)
- Yangbai (GB14)
- Xiaguan (ST7)
- Yifeng (SJ7)
With the exception of the Hegu acupoint, only the acupoints on the affected side were treated. The acupuncturist used a filiform needle, applying high speed pulling (Ti), pushing (Cha), and rotating (Nian Zhuan) techniques. Upon arrival of a deqi sensation, a needle retention time of 30 minutes was observed. Next, moxibustion was administered to the same acupoints for 5 minutes each (simultaneously on both Hegu acupoints) until the surrounding skin took on a flushed appearance. The acupuncture and moxibustion sessions were conducted once daily for 6 consecutive days with a 1 day break afterwards. The treatment cycle was repeated for a total of 4 weeks. The control group was given the following medications:
- Vitamin B1 (100 mg), Vitamin B12 (500 ug). Administered via intramuscular injection once daily, for 14 consecutive days.
- Prednisone (30 mg). Orally delivered once daily for 5 consecutive days. After 5 days, dosage was reduced to 5 mg administered once daily for 5 consecutive days.
- Vitamin B1 (10 mg), methycobal (500 ug). Orally administered 3 times daily for 14 consecutive days.
Patient progress was monitored and documented before and after treatment. Evaluation was based on the House-Brackmann Classification of Facial Function. After treatment, patients were taught how to identify facial paralysis symptoms and were requested to contact a doctor in case of facial paralysis reoccurrence. To ensure the accuracy of records, patients were contacted by phone once every 2 months to enquire about paralysis relapses. Patients were advised to consult a doctor for further diagnosis if they experienced relapses.
The study by Changsha and Yueyang hospital researchers indicates that treatment outcomes produced by acupuncture and moxibustion are superior to that of pharmaceutical medications. Based on the clinical results of the study, researchers conclude that acupuncture and moxibustion do not cause facial muscle spasms when administered during the acute phase of facial paralysis but instead improve recovery rates.
The 3 studies mentioned above share similarities. Researchers determined that acupuncture is successful for the treatment of facial paralysis. Scientific investigations demonstrate that acupuncture works in tandem with a range of other traditional Chinese and western facial paralysis treatments. Above all, acupuncture is a safe and effective method when administered by licensed acupuncturists for the treatment of facial paralysis.
References:
Wang, X., Jin, T. & Ma, S. L. (2014). Red glow with acupuncture and medication curative effect observation of 96 cases of facial paralysis. Laser Journal. 35 (2).
Cai, NS, Yu, HB & Ma, XM. (2015). Clinical observation on acupuncture therapy combined with TCM nursing intervention for patients with liver stagnation type of facial paralysis. Chinese Nursing Research. 29 (8B).
Shi, F. & Zhang, B. S. (2004). Facial Neuritis Patients Psychological Assessment: 60 Cases. Chinese General Practice. 7(15): 1061-1062.
Lin N, Lin XM, Fu L, Yan GF & Li SJ. (2014). Curative Effect of Acupuncture and Moxibustion on Facial Paralysis at Acute Period and Follow-up of Two Years. Journal of Clinical Acupuncture and Moxibustion. 30(11).
Li J, Liang FR, Yu SG et al. (2005). A large and random sampling method for acupuncture-moxibustion in the treatment of Bell’s palsy. Chinese Journal of Clinical Rehabilitation. 9(33): 97-99.
Yahho TC, Jankovic J. (2011). The mang faces of hemifacial spasm: Differential diagnosis of unilateral facial spasm [J]. Mov Disord. 26(9): 1582-1592.


