Long needle acupuncture, electroacupuncture and Xiaoxingnao acupuncture show positive treatment outcomes for both cervical spondylosis and cervical spondylotic radiculopathy.
Two recent research studies find acupuncture a highly effective and flexible method for the treatment of cervical spondylosis and cervical spondylotic radiculopathy (neck spinal and soft tissue degeneration causing nerve impingement and subsequent pain or numbness). One study from Xindu District Hospital of Traditional Chinese Medicine found long needle acupuncture to be highly effective for the treatment of cervical spondylotic radiculopathy. Another from Tianjin University of TCM determined that electroacupuncture treatment in combination with Xiaoxingnao acupuncture produces significant patient outcomes.
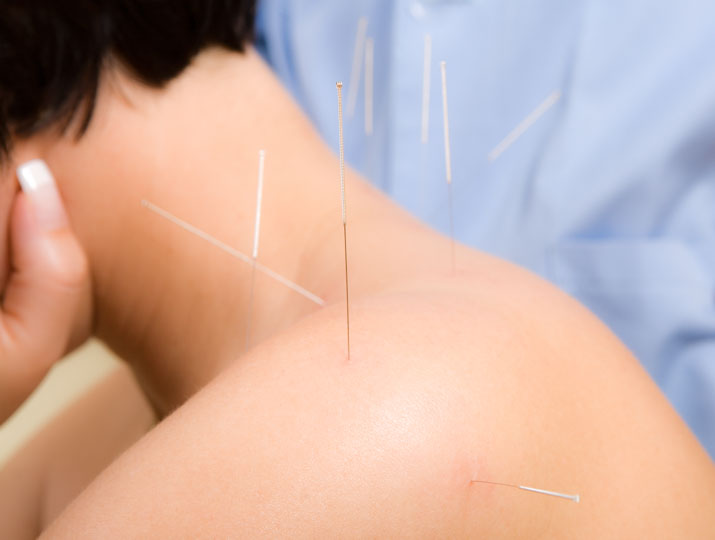
In the first study, researchers Xie et al. (Xindu District Hospital of Traditional Chinese Medicine) conducted a scientific investigation of long needle acupuncture compared with conventional acupuncture for the treatment of cervical spondylotic radiculopathy. The results demonstrate that long needle acupuncture produces superior patient outcomes. Let's take a look at the advanced procedures that produced the results. Please keep in mind that the following procedures are only appropriate for licensed acupuncturists trained in these expert techniques and procedures.
Cervical spondylotic radiculopathy is a common disease that usually affects patients between the ages of 25 and 65 years old. It is mainly caused by bone hyperplasia and hypertrophy of the intervertebral discs, vertebral joints and facet joints. Consequently, the corresponding spinal nerve roots and other nerve roots are compressed or damaged. The main symptoms of this condition include neck, shoulder, back, upper limb, and finger pain, numbness, radiculopathy, or limb and finger weakness (Yang et al., 2012).
Long needle acupuncture accelerates qi and blood circulation in the meridians and also facilitates communication between the yin and yang meridians or between multiple acupoints. For this reason, it is appropriate for the treatment of cervical spondylotic radiculopathy. The study found that long needle acupuncture demonstrates a higher efficacy rate than conventional acupuncture for the treatment of this condition.
A total of 126 patients with cervical spondylotic radiculopathy were selected for the study. They were divided into two groups: treatment group (64 patients), control group (62 patients). The treatment group underwent long needle acupuncture whereas the control group underwent conventional acupuncture treatment. Identical primary acupoints were selected for both therapies: neck Jiaji acupoints and traditional Hua Tuo Jiaji acupoints. These acupoints run in two parallel lines on either side of the spinal column and the Governing Vessel meridian, 0.5–1 cun lateral to the spinous process of each vertebrae. They function to stimulate the nerve segment corresponding to their specific locations.
For the long needle acupuncture treatment, a 3 inch acupuncture needle was held with both hands and inserted into each acupoint. For the neck Jiaji acupoints, the long needle was pointed downwards and inserted towards the seventh cervical vertebra. Upon insertion, either the Ping Bu Ping Xie (gently reinforcing and reducing) or the Xie (reducing) needle manipulation technique was applied. Needle techniques were selected depending upon the individual patient’s clinical symptoms. One acupuncture session was conducted daily for 20 days in total, in two cycles of 10 consecutive days, with a 1 to 2-day break between each cycle.
For conventional acupuncture, a 1.5 inch filiform needle was inserted into each acupoint, angled toward the midline. Upon insertion, either the Ping Bu Ping Xie or the Xie needle manipulation technique was applied, depending upon the individual patient’s clinical symptoms. One acupuncture session was conducted daily for 20 days in total, in two cycles of 10 consecutive days, with a 1 to 2 day break between each cycle. The patients receiving long needle acupuncture achieved a 95.3% total treatment effective rate, while those who received conventional acupuncture achieved an 80.6% rate. The results of this study indicate that long needle acupuncture is highly effective in treating cervical spondylotic radiculopathy, showing greater improvements in symptoms than conventional acupuncture.
In the second study, researchers Gong and Xue (Tianjin University of TCM) found that Xiaoxingnao acupuncture (a specialized acupuncture technique which effectively dredges meridians, improves blood circulation and refreshes the mind) combined with electroacupuncture on the cervical Jiaji acupoints is effective for the treatment of Vertebral artery cervical spondylosis. Vertebral artery cervical spondylosis arises from arterial oppression or damage from mechanical and dynamic factors. This leads to stenosis, which eventually decreases blood supply to the vertebral basilar artery. The main symptoms of vertebral artery cervical spondylosis include: neck and shoulder pain, dizziness, headache, cataplexy, optical conditions (e.g., fogged vision, dark spots, transient amaurosis, temporary vision defects, degenerated vision, ambiopia, visual hallucinations, blindness). In addition, bulbar paralysis and other neurological symptoms may be observed including slurred speech, dysphagia, pharyngeal reflex, choking due to backflow while drinking water, palatoplegia, voice hoarseness or facial paralysis.
The study involved a total of 60 patients with vertebral artery cervical spondylosis. They were divided into two equal groups of 30: the treatment group and the control group. Patients in the treatment group were treated with a combination of Xiaoxingnao acupuncture therapy with electroacupuncture. The control group patients received pharmaceutical medications. The clinical results of this study demonstrate that combining electroacupuncture and Xiaoxingnao acupuncture yields significantly better treatment outcomes than medications. Primary acupoints selected for the treatment group’s therapy were the following:
- Fengchi (GB20)
- Fengfu (GV16)
- Tianzhu (BL10)
- Wangu (SI4)
- Dazhui (GV14)
- Cervical Jiaji acupoints
Fengchi, Fengfu and Tianzhu acupoints were selected for their ability to reduce muscule spasms, regulate autonomic nerve functions, dilate blood vessels and improve blood supply to the brain. Wangu was selected for the treatment of headaches and neck pain. Dazhui was selected to facilitate blood flow. Finally, the cervical Jiaji acupoints were selected as local points to dredge the affected meridians (Deng et al., 2008). For the Fengchi, Fengfu, Tianzhu and Wangu acupoints, the needles were inserted 1.5 – 2 inches deep, toward the Adam’s apple. Acupoints were manipulated by rotating in small turns at a high frequency. For the Dazhui acupoint, multiple needles were inserted in various directions: upward, downward, to the left, to the right and perpendicularly (until the patient felt a sensation radiating toward the shoulder).
The cervical Jiaji acupoints were inserted perpendicularly to a depth of 1.5 – 2 inches. An electroacupuncture device was connected to the needles at the cervical Jiaji acupoints, set at 2 – 10 Hz with disperse-dense waves. Additional secondary acupoints were selected on an individual symptomatic basis as follows:
For phlegm and dampness retention:
- Fenglong (ST40)
- Yanglingquan (GB34)
For phlegm and blood stasis:
- Hegu (LI4)
- Sanyinjiao (SP6)
- Geshu (BL17)
- Zhongwan (CV12)
- Fenglong (ST40)
- Zusanli (ST36)
For accumulation of dampness and heat:
- Danshu (BL19)
- Yanglingquan (GB34)
- Neiguan (PC6)
- Shenmen (HT7)
- Fenglong (ST40)
For blood deficiency:
- Geshu (BL17)
- Xuehai (SP10)
- Zusanli (ST36)
- Sanyinjiao (SP6)
- Qihai (CV6)
For all secondary acupoints, the Ping Bu Ping Xie needle manipulation technique was applied. After needle insertion and manipulation, a needle retention time of 20 minutes was observed. One 20 minute acupuncture session was conducted daily for 2 consecutive weeks.
Patients taking medications received intravenous infusions including mannitol and safflower extract injections in addition to medications to promote blood circulation, nourish nerves, and energize the body. The medications were administered once daily for 2 consecutive weeks. The results of this study showed that patients who underwent combined Xiaoxingnao acupuncture and electroacupuncture achieved an excellent total treatment effective rate of 93.3%, while those who received conventional medications plus infusions achieved a 76.7% total treatment effective rate.
The two aforementioned clinical studies demonstrate that different types of acupuncture have varying efficacy rates for the treatment of cervical spondylosis and cervical spondylotic radiculopathy. Electroacupuncture and Xiaoxingnao acupuncture were more effective than medications. Long needle acupuncture produced greater positive patient outcomes than conventional acupuncture. This reflects the dynamic nature of acupuncture and its flexibility for the treatment of these common conditions.
References:
Xie XY, Qing S, Liao JK, Xiao Y, Liu JQ. (2013). Clinical Efficacy of Long Needle Penetration Acupuncture on Cervical Spondylotic Radiculopathy: A Clinical Observation of 64 Cases. Guiding Journal of Traditional Chinese Medicine and Pharmacology. 7(7).
Yang JX, Yu JC, Zhang JP et al. (2012). Triple Jiao acupuncture in treating cervical spondylotic radiculopathy. Chinese General Practice. 15(25): 2963-2965.
Gong XL, Xue YY. (2014). Clinical Observation of Xiaoxingnao acupuncture Combined with Electroacupuncture at Cervical Jiaji Points in Treatment of Vertebral Artery Type of Cervical Spondylosis.
Journal of Hubei University of Chinese Medicine. 16(5).
Deng LX, Wu XP, Huang W, Wu QK & Jiang GD. (2008). Electroacupuncture in treating vertebral artery type of cervical spondylosis. Journal of Hubei College of Traditional Chinese Medicine. 1.


