Acupuncture and herbal medicine improve rheumatoid arthritis patient outcomes. Qingdao Integrated Medicine Hospital (Shandong) researchers conclude that a combination of acupuncture, Chinese herbal medicine, and drug therapy is more effective than drug monotherapy. [1] Two groups were compared in a clinical study. One group received a combination of the herbal formula Wen Shen Tong Bi Tang, warm needle acupuncture, diclofenac, and methotrexate. The other group received only diclofenac and methotrexate. At 12 and 18 month follow-up assessments, patients receiving acupuncture, herbs, and drugs had significantly greater patient outcomes than patients receiving only drugs.
Rheumatoid arthritis symptoms improved significantly for patients receiving the integrative medicine protocol. In addition, objective measurements of RF (rheumatoid factor), CRP (c-reactive protein), and ESR (erythrocyte sedimentation rate) also improved significantly. For both subjective and objective factors, the addition of acupuncture and herbs improved patient outcomes.
The study included 180 patients meeting the biomedical and TCM (traditional Chinese medicine) diagnostic criteria for RA (rheumatoid arthritis). Further inclusion criteria were as follows: ages 18–65 years, RA stages 1–3, no concurrent medical conditions, and the ability to give voluntary consent.
Exclusion criteria were as follows: not meeting diagnostic criteria for RA, pregnancy, lactation, allergies to drugs used in the study, inflammatory disease (e.g., systemic lupus erythematosus, osteoarthritis, heart, liver, kidney, hematopoietic, serious primary diseases, psychiatric disorders, use of hormone therapy), inability to comply with treatment, or current participation in other trials. Patients were assigned to the acupuncture group (n=90) or the control group (n=90) by random number table, according to recruitment order, gender, age, and disease duration.
Both groups were prescribed methotrexate (10 mg weekly), taken as a single dose and accompanied by folic acid (4 mg). Both groups were also prescribed diclofenac (75mg), twice each day. In addition, patients in the acupuncture group were prescribed Wen Shen Tong Bi Tang herbal formula, which was comprised of the following ingredients:
- Sang Ji Sheng 30 mg
- Dang Gui 20 mg
- Shu Di Huang 20 g
- Du Zhong 20 g
- Gui Zhi 10 mg
- Bai Shao 20 g
- Zhi Mu 20 g
- Fu Zi 12 g
The formula was prepared at the hospital pharmacy, allowing for uniform decoction preparation. A total of 200 ml was administered daily, divided into two separate doses. Warm acupuncture was also administered at the following acupoints:
- Xiyan (MNLE16)
- Liangqiu (ST34)
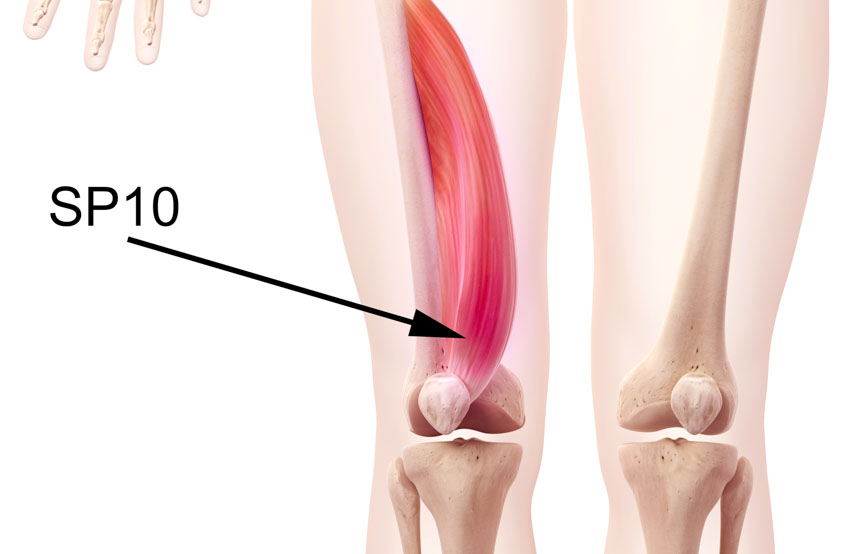
- Xuehai (SP10)
- Yanglingquan (GB34)
- Yinlingquan (SP9)
With patients in a supine position, 0.3 × 50 mm, single-use needles were inserted and manipulated to elicit deqi. Next, a 1.2 cm piece of moxa was attached to the needle handles and ignited. Once extinguished, moxibustion was repeated once more, giving a total treatment time of 15–25 minutes. Treatment was administered daily with one week constituting one course of care.
Results
Outcome measures were assessed at 6, 12, and 18 months. Outcome measures included RA symptom severity, RF (rheumatoid factor) CRP (c-reactive protein), ESR (erythrocyte sedimentation rate), SF-36 (short form 36) for quality of life (e.g., pain, physical function, blood pressure, general health, vitality, social function, emotional and mental health). Quantified RA symptoms included the number of painful joints, number of tender joints, number of swollen joints, duration of morning stiffness, and VAS (visual analog scale) scores. Mean pre-treatment symptom scores in the acupuncture group were 12.66, 12.03, 11.13, 120.20 minutes, and 8.35, respectively. In comparison, scores in the control group at the same timepoints were 12.57, 12.10, 10.95, 121.33 minutes, and 8.62.
At 6 months, symptom scores in the acupuncture group reduced to 9.28, 9.88, 8.56, 95.20 minutes, and 5.01 respectively. Scores in the drug control group were 9.37, 10.02, 8.65, 96.17 minutes, and 5.16.
At 12 months, symptom scores in the acupuncture group reduced further to 5.98, 6.01, 5.00, 52.78 minutes, and 2.11 respectively. Comparative scores in the drug monotherapy control group were 7.58, 8.10, 6.86, 53.56 minutes, and 3.27. At this timepoint, significantly greater improvements were seen in the acupuncture group across all outcome measures, except for morning stiffness duration (p<0.05).
At 18 months, symptom scores in the acupuncture group reduced further to 3.50, 3.42, 2.92, 36.46 minutes, and 1.00 respectively. Comparative scores in the control group were 5.60, 5.72, 4.75, 37.33 minutes, and 2.01. Again, significantly greater improvements were seen in the acupuncture group across all outcome measures, except for morning stiffness duration (p<0.05).
Mean pre-treatment scores for RF (RU/ml), CRP (mg/L), and ESR (mm/h) were 83.12, 35.31, and 73.92 respectively in the acupuncture group and 84.06, 36.72, 75.21 in the drug monotherapy control group. At 6 months, these scores fell to 60.35, 25.80, and 55.11 in the acupuncture group and 63.10, 27.41, and 59.67 in the control group. At 12 months, these scores improved to 41.65, 16.01, and 32.34 in the acupuncture group and 43.13, 21.33, and 45.79 in the drug control group. Finally, at 18 months, these scores had fallen further to 30.50, 9.43, and 20.95 in the acupuncture group and 32.38, 14.71, and 31.52 in the control group. Reductions in both CRP and ESR were significantly greater in the acupuncture group at 12 and 18 months (p<0.05).
The remaining outcome measures followed a similar pattern, with significantly greater improvements in all but general health, vitality, and mental health in the acupuncture group at the 12-month assessment (p<0.05). After 18 months, the acupuncture group displayed significantly greater improvements across all outcome measures (p<0.05).
The results of this study indicate that acupuncture and herbs provide significant relief from the signs and symptoms of RA and improve quality of life. The data indicates that improvements accumulate over time with the greatest improvements seen after 12 months of treatment.
Reference:
1. Liu Xiaobo, Chen Liyan, Li Aimin (2019) “A clinical study on improving the quality of life in patients with RA with the Wenshen Tongbi decoction plus warm-acupuncture” Clinical Journal of Chinese Medicine Vol.11(17) pp.84-87.


