Acupuncture plus herbs alleviates depression. Funing County People’s Hospital researchers conducted a randomized clinical trial comparing the efficacy of acupuncture plus herbs with medication therapy. The Traditional Chinese Medicine (TCM) therapy group receiving acupuncture plus herbal medicine had a 93.3% total effective rate. The pharmaceutical medication group achieved a 70% total effective rate. 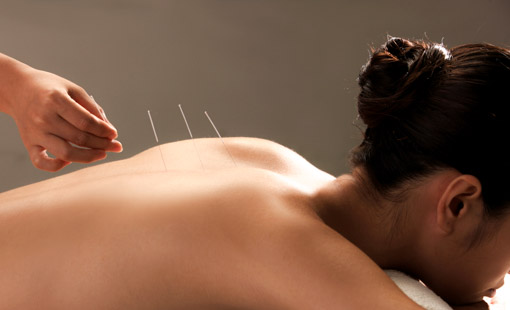
Sixty patients were randomly divided into a TCM group and a drug therapy group. The TCM group received manual acupuncture and the herbal formula Mei Gui Jie Yu Tang for oral intake. The drug therapy group received flupentixol-melitracen, a combination of an antipsychotic medication and a tricyclic antidepressant. Based on the data, the researchers note that acupuncture combined with Mei Gui Jie Yu Tang is a reliable and affordable treatment method for alleviating depression.
Acupuncture was manually applied with mild reinforcing and reducing techniques. Three acupuncture treatments were administered each week for eight weeks. Needle retention time was thirty minutes per acupuncture session and manual acupuncture techniques were applied once every fifteen minutes. Primary acupuncture point used in the study were:
- DU20, Baihui
- BL15, Xinshu
- BL18, Ganshu
- HT7, Shenmen
- DU14, Dazhui
- ST36, Zusanli
The herbal formula Mei Gui Jie Yu Tang was selected for its TCM functions of calming and balancing. Ten grams of each Chinese herbal medicine was decocted to 300 mL for oral intake twice per day:
- Me Gui Hua
- Chai Hu
- Zhi Shi
- Xiang Fu
- He Huan Pi
- Yuan Zhi
- Bai Shao
- Gan Cao
- Dan Shen
- Zhi Zi
- Jiang Huang
- Chen Pi
- Chuan Xiong
- Tian Ma
- Shi Chang Pu
Assessment tools included the Zung self-rating depression scale and the Hamilton depression scale (HAM-D). Acupuncture plus herbs achieved a 93.3% total effective rate and the medication achieved a 70% total effective rate. The acupuncture plus herbs protocol demonstrated that it is both safe and effective. 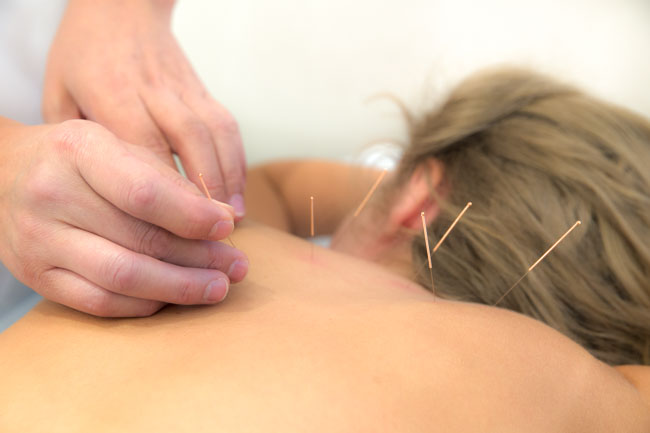
Researchers from the Tianjin University of TCM (Traditional Chinese Medicine) had similar findings to that of Gao et al. from the Funing County People’s Hospital. Their experiments reveal that adding acupuncture to a regimen of fluoxetine intake increases the total effective rate for the relief of depression by 10%. Combining acupuncture with fluoxetine intake demonstrated another very important clinical effect. Onset of clinical benefits was significantly faster when acupuncture was added to the treatment regimen. Fluoxetine, also known by the brand name Paxil, achieved a 77.05% total effective rate. The combination therapy of acupuncture plus fluoxetine achieved an 88.5% total effective rate.
The researchers measured biochemical responses and determined that acupuncture successfully regulated serum interferon (IFN-gamma) and interleukin (IL-4) levels. This confirms the work by Zheng et al. documenting that acupuncture successfully decreases IFN-gamma levels while increasing IL-4 levels. In patients with depression, there is often increased IFN-gamma levels and low IL-4 levels. The addition of acupuncture to drug therapy helped to restore normal levels while achieving successful clinical results for the relief of depression.
References:
Gao ZD, Zhang YX & Du L. (2015). Clinical Study of Meigui-jieyu decoction combined with acupuncture on depression. Journal of Anhui Traditional Chinese Hebei Journal of Traditional Chinese Medicine. 37(5).
Zhang DL. (2005). Acupuncture in treating depression. China Journal of Clinical Rehabilitation. 9(20): 217.
Lin, H., Yu, Z. F. & Kang, F. H. (2014). Th1/Th2 Balance on Depression Patients by Acupuncture Treatment Combined with Antidepressant. Journal of Clinical Acupuncture and Moxibustion. 30 (7).
Qu SS, Huang Y, Zhang ZJ, et al. A 6-week randomized controlled trial with 4-week follow-up of acupuncture combined with paroxetine in patients with major depressive disorder. J Psychiat Res 2013;47:726–32. 13 Zhang ZJ, Ng R, Man SC, et al. Dense cranial.
Chen, Junqi, Weirong Lin, Shengxu Wang, Chongqi Wang, Ganlong Li, Shanshan Qu, Yong Huang, Zhangjin Zhang, and Wei Xiao. "Acupuncture/electroacupuncture enhances anti-depressant effect of Seroxat: the Symptom Checklist-90 scores." Neural Regeneration Research 9, no. 2 (2014): 213.


