Acupuncture benefits patients with Alzheimer’s disease. Wu’an Hospital of Chinese Medicine (Hebei, China) researchers conducted a clinical trial. They conclude that a combination of acupuncture and Bu Shen Huo Xue Tang herbal formula provides significant clinical results for Alzheimer’s disease patients. Patients receiving acupuncture plus herbs experienced improvements in cognitive function and quality of life (total effective rate 84%). The drug control group had a 68% total effective rate. [1]
A total of 50 patients with Alzheimer’s disease were recruited for the study and were randomly assigned to the control group or the acupuncture group. The control group was comprised of 15 male and 10 female patients, ages 60–76 years (mean age 65.42 years), with a disease duration of 2–6 years (mean duration 4.23 years). The acupuncture group was comprised of 12 male and 13 female patients, ages 61–74 years (mean age 64.23 years), with a disease duration of 2–7 years (mean duration 4.12 years). None of the patients were suffering from serious cardiovascular or cerebrovascular disease and none were postpartum or lactating. There were no statistically significant differences in baseline characteristics between the two groups (p>0.05) at the start of the investigation.
Acupuncture, Herbs, And Drug Therapy
Patients allocated to the control group received pharmacological intervention for Alzheimer’s disease. The prescribed medications included donepezil at a dosage of 5 mg daily and nimodipine at a dosage of 30 mg, three times a day. Patients allocated to the acupuncture group received treatment at the following primary acupoints:
- Neiguan (PC6)
- Renzhong (GV26)
- Baihui (GV20)
- Sanyinjiao (SP6)
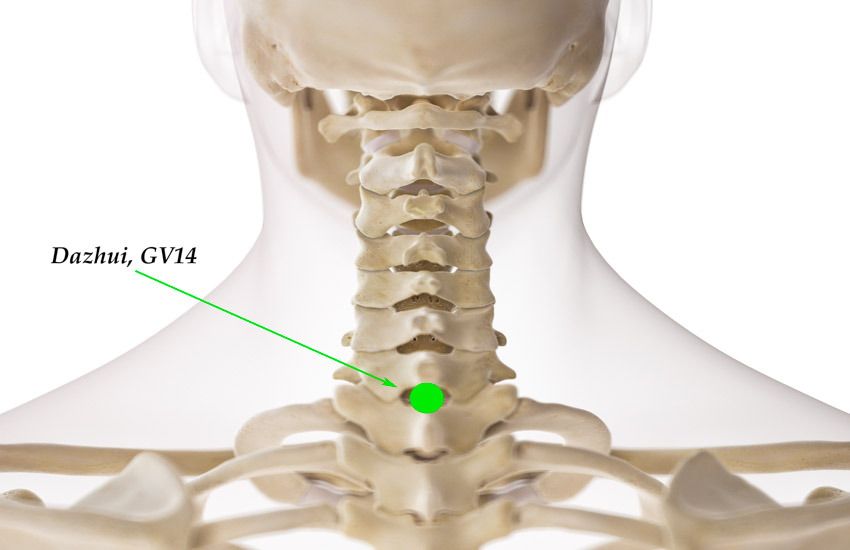
- Dazhui (GV14)
- Shenmen (HT7)
The following secondary acupoints were added for patients with a TCM diagnosis of kidney deficiency:
- Shenshu (BL23)
- Taixi (KD3)
- Yanglingquan (GB34)
Treatment was administered with each patient in a supine position. Following standard disinfection, 2-cun stainless steel filiform needles were inserted into the acupoints. Points on the scalp were inserted at a 30-degree angle, ensuring that the needle penetrated under the aponeurosis to an appropriate depth. Needles were retained for 30 minutes each acupuncture session was conducted daily. In addition, patients in the acupuncture group were prescribed Bu Shen Huo Xue Tang formula, comprised of the following herbs:
- Huang Qi 20g
- Shu Di Huang 20g
- Dan Shen 20g
- Gou Qi Zi 20g
- Du Zhong 15g
- He Shou Wu 15g
- Shi Chang Pu 10g
- Chuan Xiong 10g
- Bai Zhu 10g
- Yuan Zhi 10g
- San Qi 6g
For patients suffering from constipation, Huo Ma Ren 15g was added. For patients suffering from night-time restlessness, Suan Zao Ren 30g was added. For patients suffering from urinary frequency, Sang Piao Xiao 15g was added. The herbs were soaked in water for one hour before decocting three times for an hour each time. The resulting liquid was divided into two doses to be taken morning and evening. All patients received treatment for a total of three months.
Results
Outcome measures for the study included ADI (activities of daily living), MMSE (Mini Mental State Exam), PSP (Personal and Social Performance scale), and SF-36 (Short Form 36) scores. The total effective rate was also calculated for each group.
ADI scores are used to measure a patient’s ability to perform everyday tasks such as personal care, eating, and mobility. Lower scores are indicative of increased ability. Prior to treatment, mean ADI scores were 49.65 in the control group and 49.67 in the acupuncture group. Following three months of treatment, these scores fell to 43.23 and 40.12 respectively. Both groups saw improvements in ADI scores, but these were significantly greater in the acupuncture group (p<0.05).
The MMSE score is intended to measure a patient’s cognitive function by asking a series of questions which may be answered correctly or incorrectly. Higher scores are indicative of more correctly answered questions and, therefore, better cognitive function. Mean pre-treatment MMSE scores were 15.23 in the control group and 15.45 in the acupuncture group. Following three months of treatment, these scores increased to 18.45 and 22.56 respectively. Both groups saw improvements in MMSE scores following treatment, but were significantly greater in the acupuncture group (p<0.05).
The PSP is designed to measure a patient’s performance in areas including self-care, relationships, and behavior. Higher scores are indicative of improved performance. Mean pre-treatment PSP scores were 45.23 in the control group and 45.78 in the acupuncture group. After treatment, these scores increased to 67.45 and 79.89 respectively. Both groups saw improvements in PSP scores following treatment. These were significantly greater in the acupuncture group (p<0.05).
The SF-36 is a 36-item scale which measures quality of life, with higher scores indicative of improved quality. Mean pre-treatment SF-36 scores were 75.56 in the control group and 76.34 in the acupuncture group. After treatment, these scores increased dramatically, to 121.78 and 145.75 respectively. Although both groups saw significant improvements in SF-36 scores following treatment, improvements were significantly greater in the acupuncture group (p<0.05).
The total effective rates were calculated for each group. At the end of treatment, there were 17 effective cases in the control group, giving a total effective rate of 68%. In the acupuncture group, there were 21 effective cases at the end of treatment, giving a total effective rate of 84%. The difference in effective rates between the two groups is statistically significant (p<0.05).
The results of this study indicate that acupuncture combined with herbal medicine provides an effective treatment option for patients with Alzheimer’s disease. Acupuncture and herbs may help to improve both cognitive function and quality of life, and outperforms the medications donepezil and nimodipine.
Reference:
1. Zhang Wenshun (2019) “Analysis of the effect of acupuncture combined with traditional Chinese medicine treatment for senile dementia” World’s Latest Medicine News Digest Vol. 19(24), pp145, 147.


